ACL Tear
(Redirected from ACL Injury)
Other Names
- Anterior Cruciate Ligament Injury
- Anterior Cruciate Ligament Tear
- ACL Tear
- ACL Partial Tear
- ACL Sprain
- ACL Injury
- Tibial Spine Fracture
- Segond Fracture
- Tibial eminence avulsion fracture
Background
- This page refers to injuries to the Anterior Cruciate Ligament (ACL)
History
- 170 A.D.: Galen: First description of the cruciate ligaments in the knee[1]
- In 1895, A. W. Mayo Robson: First reported surgical repair of the ACL[2]
- Jones described the first patellar tendon ACL reconstruction technique in 1963[3]]]
Epidemiology
- ACL is the most commonly injured knee ligament
- Account for up to 64% of athletic knee injuries in cutting and pivoting sports (need citation)
- Incidence
- In the general population of approximately 1 in 3500 (need citation)
- Cost
- 120,000–200,000 ACL reconstructions (ACLRs) performed annually in the United States[4]
- Cost of around 1.7 billion US dollars annually
- Pediatric considerations
Introduction

General
- The anterior cruciate ligament (ACL) is a key stabilizing structure in the knee that prevents anterior translation of the tibia and provides rotational stability
- ACL tears commonly occur during non-contact pivoting, cutting, or sudden deceleration movements, especially in athletes
- Patients often report a “pop” at the time of injury followed by immediate swelling, instability, and difficulty bearing weight
- Diagnosis is primarily clinical using tests such as the Lachman and anterior drawer, with MRI used to confirm the injury and assess associated damage
- Management is generally surgical, although non-surgical management is an option in appropriate patients
Tear Location
- Skeletally mature athlete likely to have mid-substance tear
- Young, skeletally immature athlete more likely to have at the origin of the femur
Etiology
- Noncontact
- Majority of injuries occur during noncontact mechanism (60-70% of ACL injuries)[9]
- Typically sustained when a running or jumping athlete suddenly decelerates, changes direction (eg, cutting), pivots or lands
- Leads to rotation, lateral bending (ie, valgus stress) of the knee, anterior translation of the tibia on the femur
- Often encompass an ill-timed neuromuscular firing of structures around the knee
- Indirect contact
- Occur when a person or object strikes a part of the body other than the knee itself
- Direct contact
- Defined as injury sustained when a person or object strikes the knee directly
- Most often causing hyperextension or valgus deformation of the knee
- Example: player's foot is planted, opponent strikes him on the lateral aspect of the planted leg
- High speed trauma
- Uncommon but can happen from MVC
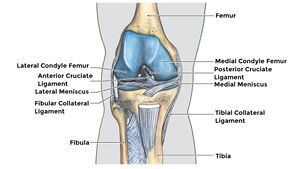
Anatomy of the Anterior Cruciate Ligament
- Extends from the lateral femoral condyle to the anterior medial aspect of the tibia[10]
- Acts as primary passive restraint to anterior translation of the tibia on the femur
- The bands of the ACL act as a biomechanical restraint in rotational and frontal planes
- It assists with knee stability during running, jumping, cutting or pivoting.
Associated Injuries
- Epidemiology[11][12]
- Approximately 76-79% of ACL injuries have a co-occurring internal derangement of the knee
- Most commonly: medial meniscus (57%), lateral meniscus (25%), medial collateral ligament (41%)
- Bone bruising/ contusion is present in 92% of patients
- Meniscus Injury
- Osteochondral Defect
- Multiligament Knee Injury
- PCL Injury
- MCL Injury
- LCL Injury
- Posterolateral Corner Injury
- Bone contusion, less commonly fracture
Anatomy of the Anterior Cruciate Ligament
- The anterior cruciate ligament (ACL) originates from the posteromedial aspect of the lateral femoral condyle and inserts onto the anterior intercondylar area of the tibia [13]
- It is composed of two functional bundles—the anteromedial (AM) and posterolateral (PL) bundles—which are tensioned differently throughout knee flexion and extension to provide dynamic stability [14]
- The ACL is primarily responsible for preventing anterior translation of the tibia relative to the femur and also contributes to rotational stability of the knee joint [15]
- Vascular supply is mainly derived from the middle genicular artery, and innervation includes mechanoreceptors that contribute to proprioception [16]
- The ligament is intra-articular but extrasynovial, meaning it lies within the joint capsule but is surrounded by synovial membrane rather than bathed directly in synovial fluid [17]
Risk Factors
- Female
- Male
- Tend to injure dominant/ kicking leg (need citation)
- ACL Tears by Sport (Gornitzky et al) [20]
- Football (0.089 per 1000 exposures)
- Lacrosse (0.058)
- Soccer (0.040)
- Basketball (0.024)
- Wrestling (0.021)
- Additional sports with higher risk
- Alpine skiing
- Tennis
- Anatomic
- Obesity
- Patella Alta
- Increasing lateral tibial posterior slope (LTPS)[21]
- Increased Q-angle
- Ligamentous Laxity
- Neuromuscular control
- Increased risk for ACL injuries[22]
- Ligament dominance
- Quadriceps dominance
- Leg dominance
- Trunk dominance
- Female athletes
- Increased risk with dynamic valgus position, abduction of lower extremities
- Dynamic Valgus Landing
- Increased risk for ACL injuries[22]
Differential Diagnosis
Differential Diagnosis Knee Pain
- Fractures
- Dislocations & Subluxations
- Patellar Dislocation (and subluxation)
- Knee Dislocation
- Proximal Tibiofibular Joint Dislocation
- Muscle and Tendon Injuries
- Ligament Pathology
- Arthropathies
- Bursopathies
- Patellofemoral Pain Syndrome (PFPS)/ Anterior Knee Pain)
- Neuropathies
- Other
- Bakers Cyst (Popliteal Cyst)
- Patellar Contusion
- Pellegrini Stieda Syndrome
- Parameniscal Cyst
- Pediatric Considerations
- Patellar Apophysitis (Sinding-Larsen-Johnansson Disease)
- Patellar Pole Avulsion Fracture
- Tibial Tubercle Avulsion Fracture
- Tibial Tuberosity Apophysitis (Osgood Schalatters Disease)
- Proximal Tibial Metaphyseal Fracture
- Proximal Tibial Physeal Injury
Clinical Features

History
- Careful description of mechanism of injury
- Patients will often describe sudden changes in the direction of movement, rapid stopping, jumping and landing abnormally
- Less commonly a direct blow to the lateral knee
- Patients usually feel a "pop"
- Will describe a buckling sensation
- Will also endorse pain, typically "deep"
- Also swelling, loss of range of motion and difficulty ambulating
- Will endorse instability, knee "giving out"
- Causes of instability include squatting, pivoting, lateral movement, walking down stairs
Physical Exam: Physical Exam Knee
- Gait: Quadriceps avoidance (does not actively extend knee)
- Very important to compare to unaffected knee
- Joint effusion: ~70% of patients with acute knee and hemarthrosis have ACL tear[24]
- Note presence and degree of effusion may limit exam
- Range of motion is typically restricted with a resting position of 20-30° knee flexion
- There may be tenderness along the tibial plateau
- If there is a tibial spine fracture, there may be a block to full extension
Special Tests
- Anterior Drawer: Patient supine, Hips flexed to 45°, knee flexed to 90°, tibia is translated anterior
- Posterior Drawer Test: be certain your anterior drawer is not mistaken for a PCL injury
- Lachmans Test: Tibia is translated anteriorly with patient supine, knee flexed to 20-30°
- Pivot Shift Test: knee in extension, hip flexed to 20-30°, internally rotate tibia, valgus stress the knee
- Lever Test: Knee extended, fist behind tibia, downward pressure on femur
- Forced Active Buckling Sign: bring knee into extension while applying a valgus stress to the knee
- KT-1000: useful to quantify anterior laxity
Evaluation



Radiographs
- Standard Radiographs Knee
- Screening tool in the setting of suspected ACL injury
- Typically normal
- A joint effusion may be seen laterally
- Segond Fracture
- Avulsion fracture at the lateral aspect of the proximal tibia
- Attachment site of the lateral collateral ligament and/or biceps femoris tendon
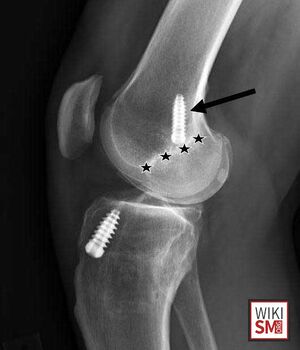
- Tibial Spine Fracture
- Fleck of bone off the center of tibial plateau that appears avulsed
- Optimal beam projection: AP with 5° caudad tilt matching the slope of the proximal tibia[26]
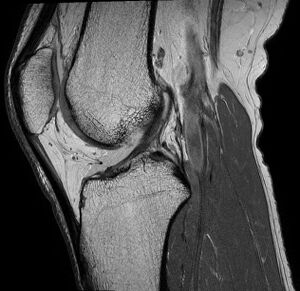
MRI
- Imaging modality of choice in the setting of suspected ACL injury
- Primary Findings
- Edema
- Increased signal (T2 weighted, proton density images)
- Discontinuity of the fibers
- Change in the expected course of the ACL
- Tears usually occur within the midportion of the ligament
- Secondary Findings
- Bone marrow edema/ contusion
- Joint effusion
- Segund Fracture (discussed above)
- Without contrast
- Sensitivity 86%
- Specificity 95%
- Arthrogram (rarely used)
- Sensitivity 92-100%
- Specificity 95-100%
Ultrasound
- Can be used to aid in the diagnosis
- Ultrasound is best at detecting complete ACL rupture
- Sensitivity is likely more limited than MRI.
- Meta-analysis[27]
- Sensitivity: 90.0% (95% CI: 77–96)
- Specificity: 97% (95% CI: 90–99)
- LR+: 31.08 (95% CI: 8.75–110.41)
- LR-: 0.11 (95% CI: 0.05–0.24)
- Post-test probability: 89% (3%)
- Diagnostic OR: 288.81 (95% CI: 78.51–1062.48)
Classification
- No current widely accepted classification system exists
Management
Prevention
- Neuromuscular control
- Increase dynamic knee stability translates to decreased incidence of noncontact ACL injury in female athletes
- Improve pre- and mid-stance neuromuscular activation patterns, decrease joint motion and protect the ACL
- Posterior chain muscle group
- Screening
- Microsoft kinect can be used for screening dynamic valgus during drop vertical jump test[30]
Nonoperative
- Indications
- Patients who are not good surgical candidates
- Low demand patients with decreased laxity
- Recreational athlete not participating in cutting/pivoting activities
- Minimally displaced tibial spine fracture
- Treatment includes
- Physical Therapy
- Lifestyle and activity modification
- Potentially Hinged Knee Brace
Operative
- Indications
- Vast majority of young, healthy adults
- Displaced tibial spine fracture
- Technique
- ACL Repair
- ACL Reconstruction
- ACL revision reconstruction
- Reconstruction sources
- Hamstring Tendon (HT)
- Bone-patellar Tendon-bone (BPTB)
- Quadriceps Tendon (QT)
- Double vs single bundle
- Double bundle reconstructs AM, PL bundles to more closely reproduce native knee anatomy
- Single bundle is used in smaller tibial insertions, severe bone bruising, arthritic changes or open physes
- Biologic agents
- Increasing interest in using biologic agents to augment repair or to treat stable partial tears
- A few small studies suggest Platelet Rich Plasma may promote graft maturation, however this is controversial
- The use of Stem Cell Therapy is highly debated and poorly understood
Rehab and Return to Play
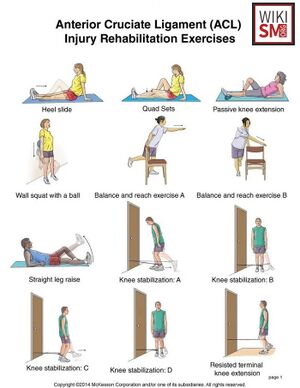
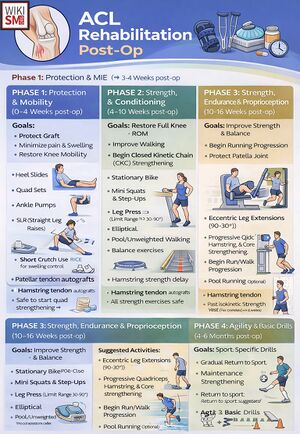
Rehabilitation
- General
- No consensus regarding most effective rehabilitation program
- General modalities and approach
- Cryotherapy (ice)
- Gravity-assisted motion or continuous passive motion (constant mechanical movement by a machine)
- Protective bracing
- Electrical neuromuscular stimulation
- Exercises (i.e., isometric, isotonic, and isokinetic) aimed at strengthening, balance, proprioception
- Mitigation of the inflammatory response
3 Stage Approach
- Acute
- Used both following acute injury, immediate postoperative period
- Goal: restore range of motion, maintain quadriceps strength, reduce inflammation
- Recovery
- Goal: improving lower limb muscle strength and functional stability
- Typically lasts 3–6 weeks
- Functional Phases
- Begins 6 weeks postinjury or postoperatively
- Goal: return the patient to his or her previous levels of function/activity
- Goal: reduce the risk of re-injury
ACL Tear Rehab Program PDFs
- Physical Therapy ACL Partial Tear PDF
- ACL Rehabilitation Protocol PDF
- ACL Nonoperative Management Exercise Program PDF
- ACL Post Op Rehab PDF
Return to Play/Work
- General
- No clear consensus on return to play guidelines
- Premature return to play associated with graft failure, contralateral ACL tear
- Recent trends favor a decelerated rehabilitation protocol with consideration of return to play in the realm of 8–12 months
- Set of criteria for return to play
- 8-12+ months from time from surgery
- Absence of pain and effusion
- Knee range of motion comparable to the contralateral limb
- Negative Lachman or pivot shift test
- Successful performance of hop tests at >85%–90% the performance of the contralateral limb
- Jump and landing tasks such as the drop vertical jump without evidence of dynamic valgus
Prognosis and Complications
Prognosis
- Nonoperative management
- Tolerated poorly by young active adults, skeletal immature
- Can lead to instability, chondral and meniscal injuries
- Cochrane review compared surgical vs nonsurgical management[31]
- No difference between surgery and conservative treatment in patient-reported knee scores at 2 and 5 years
- However, in conservative group, 39% of patients had surgery at 2 years and 51% at 5 years.
- Early vs delayed reconstruction
- Shelbourne at al showed delayed (8-21 days) was superior to early (0-7) days reconstruction for quadriceps strength, terminal knee extension[32]
- For this reason, there is a growing trend to use preoperative rehabilitation emphasizing quadriceps strength, knee range of motion
- Concomitant meniscal repair
- Saltzman et al found meniscal allograft transplantation (MAT) can provide significant improvements in clinical outcomes and enhancement in objective knee stability[33]
- Early return to play
- Increased risk of graft failure[34]
- Increased risk of injury to contralateral ACL
Complications
- Intra-operative
- Graft-tunnel mismatch
- Posterior wall blowout
- Post-operative complications
- Re-tear/ graft failure
- Failure rates as high as 14% (adults), 28% (males under 18)[35]
- May occur due to
- Tunnel malposition
- Inadequate graft fixation, hardware failure
- Graft-screw divergence >30°
- Attritional graft failure
- Graft less then 8mm in width
- Intra-articular femoral bone plug dislodgement
- Missed diagnosis of concomitant ligamentous injuries
- Over-aggressive or improper rehab
- Increased risk
- Reduced risk
- Contralateral ACL tear
- As high as 8% during 12 years follow up[38]
- Chronic complications
- Meniscal Tear
- Not necessarily present on initial injury but occurs due altered biomechanics of knee
- Chondromalacia
- Knee Osteoarthritis
- Arthrofibrosis
- Most commmon complication following ACL repair
- Altered knee kinematics and gait
- Muscle Weakness
- Reduced functional performance
- Inability to return to sport
- Loss of range of motion
- Infrapatellar contracture syndrome
- Patella Tendon Rupture
- Reflex Sympathetic Dystrophy
- Patellar Fracture
- Tunnel osteolysis
- Local nerve irritation
- Cyclops lesion
- Meniscal Tear
See Also
Internal
External
- Sports Medicine Review Knee Pain: https://www.sportsmedreview.com/by-joint/knee/
- https://mededcases.com/acl-anterior-cruciate-ligament-tear/
References
- ↑ Galen. De Usu Partium Corporis Humani.
- ↑ Robson AW. “Ruptured Crucial Ligaments and Their Repair.” Ann Surg. 1895.
- ↑ Jones KG. “Reconstruction of the Anterior Cruciate Ligament.” J Bone Joint Surg Am. 1963.
- ↑ 7. Kim S, Bosque J, Meehan JP, Jamali A, Marder R. Increase in outpatient knee arthroscopy in the United States: A comparison of national surveys of ambulatory surgery, 1996 and 2006. J Bone Joint Surg Am. 2011;93:994–1000
- ↑ Scrimshire, A. B., et al. "Management and outcomes of isolated paediatric tibial spine fractures." Injury 49.2 (2018): 437-442.
- ↑ Gans, Itai, Keith D. Baldwin, and Theodore J. Ganley. "Treatment and management outcomes of tibial eminence fractures in pediatric patients: a systematic review." The American Journal of Sports Medicine 42.7 (2014): 1743-1750.
- ↑ Rohen, Johannes Wilhelm, Chihiro Yokochi, and Elke Lütjen-Drecoll. Color atlas of anatomy: a photographic study of the human body. Schattauer Verlag, 2006.
- ↑ Case courtesy of Andrew Dixon, Radiopaedia.org, rID: 22993
- ↑ Boden, Barry P., et al. "Mechanisms of anterior cruciate ligament injury." Orthopedics 23.6 (2000): 573-578.
- ↑ Kiapour AM, Murray MM. Basic science of anterior cruciate ligament injury and repair. Bone Joint Res. 2014;3:20–31
- ↑ Cristiani, Riccardo, et al. "High prevalence of associated injuries in anterior cruciate ligament tears: A detailed magnetic resonance imaging analysis of 254 patients." Skeletal Radiology (2024): 1-11.
- ↑ Gracia, Gauthier, et al. "Epidemiology of combined injuries of the secondary stabilizers in ACL-deficient knees: medial meniscal ramp lesion, lateral meniscus root tear, and ALL tear: a prospective case series of 602 patients with ACL tears from the SANTI Study Group." The American Journal of Sports Medicine 50.7 (2022): 1843-1849.
- ↑ Moore, Keith L., et al. Clinically Oriented Anatomy. 8th ed., Wolters Kluwer, 2018.
- ↑ Standring, Susan, editor. Gray’s Anatomy: The Anatomical Basis of Clinical Practice. 42nd ed., Elsevier, 2021.
- ↑ Moore, Keith L., et al. Clinically Oriented Anatomy. 8th ed., Wolters Kluwer, 2018.
- ↑ Standring, Susan, editor. Gray’s Anatomy: The Anatomical Basis of Clinical Practice. 42nd ed., Elsevier, 2021.
- ↑ Netter, Frank H. Atlas of Human Anatomy. 7th ed., Elsevier, 2019.
- ↑ Prodromos, Chadwick C., et al. "A meta-analysis of the incidence of anterior cruciate ligament tears as a function of gender, sport, and a knee injury–reduction regimen." Arthroscopy: The Journal of Arthroscopic & Related Surgery 23.12 (2007): 1320-1325.
- ↑ DeFrancesco, Christopher J., et al. "Challenges in the management of anterior cruciate ligament ruptures in skeletally immature patients." JAAOS-Journal of the American Academy of Orthopaedic Surgeons 26.3 (2018): e50-e61.
- ↑ Gornitzky AL, Lott A, Yellin JL, Fabricant PD, Lawrence JT, Ganley TJ. Sport-Specific Yearly Risk and Incidence of Anterior Cruciate Ligament Tears in High School Athletes: A Systematic Review and Meta-analysis. Am J Sports Med. 2016 Oct;44(10):2716-2723. Epub 2015 Dec 11.
- ↑ Christensen JJ, Krych AJ, Engasser WM, Vanhees MK, Collins MS, Dahm DL, et al. Lateral tibial posterior slope is increased in patients with early graft failure after anterior cruciate ligament reconstruction. Am J Sports Med. 2015;43:2510–4.
- ↑ Hewett TE, Ford KR, Hoogenboom BJ, Myer GD. Understanding and preventing ACL injuries: Current biomechanical and epidemiologic considerations - Update 2010. N Am J Sports Phys Ther. 2010;5:234–51
- ↑ Almoallim, Hani, et al. "Approach to Musculoskeletal Examination." Skills in Rheumatology (2021): 17-65.
- ↑ Maffulli, N., et al. "Acute haemarthrosis of the knee in athletes. A prospective study of 106 cases." The Journal of Bone and Joint Surgery. British volume 75.6 (1993): 945-949.
- ↑ Fernandes, Levi Reina, et al. "Combined ACL reconstruction and Segond fracture fixation fails to abolish anterolateral rotatory instability." Case Reports 2018 (2018): bcr-2018.
- ↑ Egol, Kenneth, Kenneth J. Koval, and Joseph D. Zuckerman. Handbook of fractures. Lippincott Williams & Wilkins, 2012.
- ↑ Wang, Jianhong, et al. "The role of ultrasonography in the diagnosis of anterior cruciate ligament injury: a systematic review and meta-analysis." European Journal of Sport Science 18.4 (2018): 579-586.
- ↑ Stone EE, Butler M, McRuer A, Gray A, Marks J, Skubic M, et al. Evaluation of the Microsoft Kinect for screening ACL injury. Conf Proc IEEE Eng Med Biol Soc. 2013;2013:4152–5.
- ↑ Hewett TE, Myer GD, Ford KR, Paterno MV, Quatman CE. Mechanisms, prediction, and prevention of ACL injuries: Cut risk with three sharpened and validated tools. J Orthop Res. 2016;34:1843–55.
- ↑ Gray AD, Marks JM, Stone EE, Butler MC, Skubic M, Sherman SL. Validation of the Microsoft Kinect as a portable and inexpensive screening tool for identifying ACL injury risk. Orthop J Sports Med. 2014;2(2 Suppl)
- ↑ Monk AP, Davies LJ, Hopewell S, Harris K, Beard DJ, Price AJ, et al. Surgical versus conservative interventions for treating anterior cruciate ligament injuries. Cochrane Database Syst Rev. 2016;4:CD011166.
- ↑ Shelbourne KD, Foulk DA. Timing of surgery in acute anterior cruciate ligament tears on the return of quadriceps muscle strength after reconstruction using an autogenous patellar tendon graft. Am J Sports Med. 1995;23:686–9
- ↑ Saltzman BM, Meyer MA, Weber AE, Poland SG, Yanke AB, Cole BJ, et al. Prospective clinical and radiographic outcomes after concomitant anterior cruciate ligament reconstruction and meniscal allograft transplantation at a mean 5-year followup. Am J Sports Med. 2017;45:550–62.
- ↑ Ellman MB, Sherman SL, Forsythe B, LaPrade RF, Cole BJ, Bach BR, Jr, et al. Return to play following anterior cruciate ligament reconstruction. J Am Acad Orthop Surg. 2015;23:283–96.
- ↑ Webster KE, Feller JA. Exploring the high reinjury rate in younger patients undergoing anterior cruciate ligament reconstruction. Am J Sports Med. 2016;44:2827–32.
- ↑ Inderhaug E, Raknes S, Østvold T, Solheim E, Strand T. Increased revision rate with posterior tibial tunnel placement after using the 70-degree tibial guide in ACL reconstruction. Knee Surg Sports Traumatol Arthrosc. 2017;25:152–8
- ↑ Parkinson B, Robb C, Thomas M, Thompson P, Spalding T. Factors that predict failure in anatomic single-bundle anterior cruciate ligament reconstruction. Am J Sports Med. 2017;45:1529–36.
- ↑ 38.0 38.1 Ho B, Edmonds EW, Chambers HG, Bastrom TP, Pennock AT. Risk factors for early ACL reconstruction failure in pediatric and adolescent patients: A review of 561 cases. J Pediatr Orthop. 2016
- ↑ Ponce BA, Cain EL, Jr, Pflugner R, Fleisig GS, Young BL, Boohaker HA, et al. Risk factors for revision anterior cruciate ligament reconstruction. J Knee Surg. 2016;29:329–36.
Created by:
John Kiel on 7 July 2019 05:43:30
Authors:
Last edited:
2 April 2026 11:19:35
Categories: