De Quervains Tenosynovitis
(Redirected from De Quervain's Tenosynovitis)
Other Names
- Washerwoman's Sprain or Strain
- Stenosing Tenosynovitis
- De Quervain's Tenosynovitis (DQTS)
- de Quervain syndrome
- De Quervain’s disease
- De Quervain’s tendinitis
- De Quervain’s stenosing tenosynovitis
- Radial styloid tenosynovitis
- First dorsal compartment tenosynovitis
- Texting thumb
- Gamer’s thumb
- Mommy thumb
Background
- This page refers to stenosing tenosynovitis of the first dorsal (extensor) compartment of the wrist
History
- Named after Swiss surgeon Fritz De Quervain[1]
Epidemiology
- Second most common entrapment tendinopathy of hand behind Trigger Finger (need citation)
- More commonly occurs in women with a peak age between 40 and 59[2]
- Female-to-male ratio of approximately 2.6:1
- Overall prevalence is estimated at 0.5% in men and 1.3% in women[3]
Introduction
General
- Presents with subacute dorsal/radial thumb and wrist pain
- Generally associated with overuse, although direct trauma can also be a source
- Diagnosis is clinical but can be confirmed with MRI and ultrasound
- Treatment is nonsurgical including NSAIDS, brace, physical therapy, activity modification and injections
Etiology
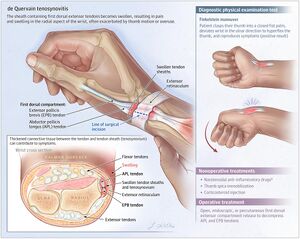
- The extensor retinaculum creates a fibroosseus tunnel, securing the APL and EPB tendons
- Thickening of the retinaculum from repetitive microtrauma restricts normal gliding
- Subsequently, there is swelling, thickening, remodeling and ultimately stenosing of the sheath
- Note this is not generally considered to be an inflammatory process
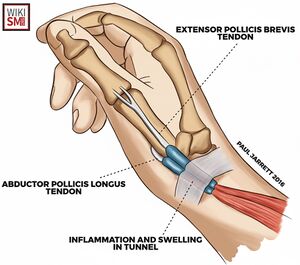
Anatomy of the First Dorsal Compartment
- Located lateral to the radial styloid process
- Contains: extensor pollicis brevis (EPB) abductor pollicis longus (APL) tendons
- In about 1/3 of patients, the EPB tendon is compartmentalized off from the APL tendon[5]
Risk Factors
Demographic
- Female > Male
- Middle Age
- Black Women
Occupational/ Activity risk factors
- Mothers and childcare workers
- Secretarial occupations
- Nursing
- Repetitive, forceful, or ergonomically stressful manual work
- Smartphone use
Other
- Pregnancy[6]
- Diabetes Mellitus
- Rheumatoid Arthritis
- Lupus
- Hypothyroidism
Differential Diagnosis
DDx Finger and Hand Pain
- Fractures
- Dislocations
- Tendinopathies
- Extensor Tendon Injuries of the Hand
- Central Slip Extensor Tendon Injury
- Flexor Tendon Injuries of the Hand
- Boutonniere Deformity
- Swan Neck Deformity
- Jersey Finger
- Mallet Finger
- Trigger Finger
- De Quervains Tenosynovitis
- Volar Plate Avulsion Injury
- Sagittal Band Injury
- Mannerfelt Lesion (FPL Rupture)
- Ligament Injuries
- Neuropathies
- Arthropathies
- Nail Bed Injuries
- Pediatric Considerations
- Other
DDx Wrist Pain
- Fractures
- Dislocations
- Wrist Dislocation (Radiocarpal and/or Ulnocarpal)
- Carpometacarpal Joint Dislocation
- Distal Radioulnar Joint Dislocation
- Lunate Dislocation
- Perilunate Dislocation
- Instability & Degenerative
- Tendinopathies & Ligaments
- Neuropathies
- Pediatric Considerations
- Distal Radial Epiphysitis (Gymnast's Wrist)
- Torus Fracture
- Arthropathies
- Cartilage
- Vascular
- Other
Clinical Features


History
- Patients typically report gradual onset of pain in thumb and wrist
- Worse with movement
- They report pain specifically over the radial styloid
- Symptoms can be bilateral
Examination: Physical Examination Wrist
- They will be tender at some point along the tendon distribution, most commonly at radial styloid
- Triggering or crepitus may be appreciated
- Range of motion, neurovascular exam typically normal
Special Tests
- Finkelsteins Test: is positive (pain with passive ulnar deviation)
- Eichhoffs Test: Also typically positive
- WHAT Test: Wrist Hyperflexion and Abduction of the Thumb
Evaluation
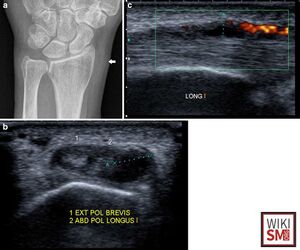

Radiographs
- Standard Radiographs Wrist, Standard Radiographs Hand
- Standard for screening, may identify other etiology of symptoms
- Typically normal
- Can show soft tissue swelling, periosteal reaction
Ultrasound
- Often diagnostic if clinical uncertainty exists
- Findings
- Will show edema or thickening of tendons
- Increased fluid within the first extensor compartment
- Thickening of retinaculum
- "Hypoechoic Halo Sign": peritendous subcutaneus edema
MRI
- Sensitive and specific for De Quervain's
- Helpful to evaluate for intertendinous septum, which increases likelihood of surgical intervention
- Findings
- Increased fluid within tendon sheath
- Debris within sheath
- Thickened retinaculum
- Peritendinous subcutaneus edema and contrast enhancement
Classification
- Not applicable
Management

Goals
- Pain reduction
- Restoration of function
- Prevention of recurrence
Nonoperative
- Indications
- Vast majority of cases
- Conservative treatment is very effective in treating this condition
- Medications including NSAIDS
- First Dorsal Compartment Injection
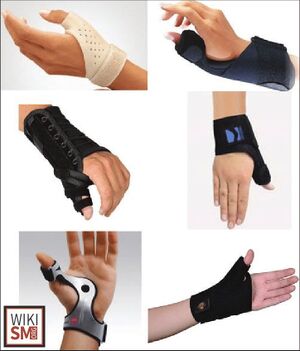
- Thumb Spica Splint or thumb spica brace
- Physical Therapy
Operative
- Indications
- Refractory cases
- Technique
- Surgery entails release of 1st dorsal compartment
- Intertendinous septum between APL And EPB increases likelihood of intervention
Rehab and Return to Play
Rehabilitation
- General
- Acute phase: gentle massage therapies, range of motion
- Subacute phase: stretching and progressive strengthening
- Return to function: functional strengthening, ergonomic training, return to work/play
- Physical therapy modalities to consider
- Paraffin Bath
- Laser Therapy[14]
- Therapeutic ultrasound
Return to Play/ Work
- There are no high quality, sport specific RTP protocols
- ACSM RTP Criteria[15]
- Complete pain resolution
- Restoration of normal strength and range of motion
- Ability to perform sport-specific skills
- Psychosocial readiness
- Stepwise RTP example
- Immobilization/rest phase (3–4 weeks) with thumb spica splinting[16]
- Gradual reintroduction of pain-free range-of-motion and strengthening exercises[15]
- Progression to sport-specific drills and functional testing
- Full return to play only when the athlete is pain-free, with normal strength and function, and poses no risk to self or others
Complications and Prognosis
Prognosis
- General
- Favorable, with most patients achieving symptom resolution and functional recovery
- Usually can improve within weeks to a few months with conservative therapy
- Nonsurgical
- Surgery
- Not typically indicated unless conservative therapy fails
- Surgical release has a success ate up to 95% (need citation)
Complications
- Persistent/ Chronic pain
- Functional impairment
- Reduction in grip strength
- Limited thumb/wrist range of motion
- Impairment in activities of daily living
- Superficial radial nerve injury
- Subluxation
- Neuroma
- Complex Regional Pain Syndrome
See Also
Internal
External
References
- ↑ Ahuja, Naveen K., and Kevin C. Chung. "Fritz de Quervain, MD (1868–1940): stenosing tendovaginitis at the radial styloid process." The Journal of hand surgery 29.6 (2004): 1164-1170.
- ↑ 2.0 2.1 Currie, Kelly Bettina, Kashyap Komarraju Tadisina, and Susan E. Mackinnon. "Common hand conditions: a review." Jama 327.24 (2022): 2434-2445.
- ↑ Hassan, Kareem, et al. "De Quervain tenosynovitis: an evaluation of the epidemiology and utility of multiple injections using a national database." The Journal of Hand Surgery 47.3 (2022): 284-e1.
- ↑ Image courtesy of https://www.ntxortho.com/, "De Quervain’s Tenosynovitis"
- ↑ Motoura H, Shiozaki K, Kawasaki K. Anatomical variations in the tendon sheath of the first compartment. Anat Sci Int. 2010 Sep;85(3):145–151. Epub December 29, 2009.
- ↑ Wolf, Jennifer Moriatis, Rodney X. Sturdivant, and Brett D. Owens. "Incidence of de Quervain's tenosynovitis in a young, active population." The Journal of hand surgery 34.1 (2009): 112-115.
- ↑ Skinner, Thomas M. "Intersection syndrome: the subtle squeak of an overused wrist." The Journal of the American Board of Family Medicine 30.4 (2017): 547-551.
- ↑ Goel, Ritu, and Joshua M. Abzug. "de Quervain's tenosynovitis: a review of the rehabilitative options." Hand 10.1 (2015): 1-5.
- ↑ Vanhoenacker, Filip M., et al. "Pseudotumoural soft tissue lesions of the hand and wrist: a pictorial review." Insights into imaging 2.3 (2011): 319-333.
- ↑ Case courtesy of Dr Maulik S Patel, Radiopaedia.org, rID: 51160
- ↑ Novikov, A. V., M. A. Shchedrina, and S. V. Petrov. "De Quervain’s disease (etiology, pathogenesis, diagnosis and treatment). Part II." NN Priorov Journal of Traumatology and Orthopedics 26.4 (2019): 55-68.
- ↑ Sawaizumi T, Nanno M, Ito H. De Quervain's disease: efficacy of intra-sheath triamcinolone injection. Int Orthop. 2007;31 (2): 265-8. doi:10.1007/s00264-006-0165-0
- ↑ Harvey FJ, Harvey PM, Horsley MW. De Quervain’s disease: surgical or nonsurgical treatment. J Hand Surg. 1990;15A:83–7.
- ↑ Chongkriengkrai, Tanach, et al. "Effectiveness of high-intensity laser application combined with splinting and therapeutic exercise in subacute de Quervain’s tenosynovitis: A pilot study." Lasers in Medical Science 38.1 (2023): 229.
- ↑ 15.0 15.1 Herring, Stanley A. "The team physician and return-to-play issues: a consensus statement." Medicine & Science in Sports & Exercise 34.7 (2002): 1212-1214.
- ↑ Chong, Han Hong, et al. "Advancements in de Quervain tenosynovitis management: a comprehensive network meta-analysis." The Journal of Hand Surgery 49.6 (2024): 557-569.
- ↑ Chongkriengkrai, Tanach, et al. "Effectiveness of high-intensity laser application combined with splinting and therapeutic exercise in subacute de Quervain’s tenosynovitis: A pilot study." Lasers in Medical Science 38.1 (2023): 229.
- ↑ Challoumas, Dimitris, et al. "Management of de Quervain tenosynovitis: a systematic review and network meta-analysis." JAMA Network Open 6.10 (2023): e2337001-e2337001.
Created by:
John Kiel on 11 June 2019 01:53:32
Authors:
Last edited:
16 October 2025 19:38:36
Categories:

