Peroneal Tendon Injuries
Other Names
- Peroneal Tendon Disorders
- Peroneal Tendinopathy
- Peroneal Tenosynovitis
- Peroneal tendon subluxation
- Peroneal tendon dislocation
- Peroneal tendon split
- Peroneal tendon tear
- Peroneal tendinosis
- Superior Peroneal Retinaculum (SPR) Injury
Background
- This page refers to disorders of the Peroneal Tendons
- This includes tendinopathies, subluxation, dislocation and tearing
History
- 1803: The first peroneal tendinopathy was a subluxation described my Monteggia[1]
- 1924: First description of an isolated split of the peroneal tendon[2]
- 1932: Operative treatment of chronic dislocation of peroneal tendons[3]
- 1934: Burman described 3 regions of peroneal tendons associated with increased incidence of tenosynovitis[4]
Epidemiology
- Only 60% of peroneal tendon disorders are accurately diagnosed at the first clinical evaluation[5]
- Most commonly seen young active patients (need citation)
- Tears
Introduction
General
- Often missed cause of lateral ankle pain
Etiology
- Acute
- Sudden contraction of the peroneal muscle group
- Inversion Ankle injury
- Chronic
- History of acute injury
- Tendon rubbing over posterolateral fibula
- Chronic lateral ankle instability
- Anatomic variants: abnormal fibular retromalleolar groove, hindfoot alignment or cavus foot
Peroneal Tendonitis
- Characterized by gradual onset of pain, swelling, warmth of the posterolateral ankle
- Lateral ankle instability can lead to laxity
- Increased motion of the tendons around the fibula with stretched superior peroneal retinaculum
- Low lying peroneus brevis muscle belly having to go through the narrow tendon sheath
Peroneal Tendon Subluxation
- Acute instability can be
- Rupture of the superior peroneal retinaculum (SPR)
- Fibular groove avulsion
- Chronic subluxation
- Associated with fibular groove flattening and laxity of the superior retinacular retinaculum or ligament
Peroneal Tendon Tear
- General
- Occurs at the musculotendinous junction
- May be acute, vast majority are chronic[7]
- Most tears are longitudinal and result from chronic subluxation over the distal fibula
- Often related to a sentinel event which is remote relative to patient presentation
- Location
- Majority of tears at tip of fibula, bony prominence where pressure is applied against tendon
- This suggests most tears are mechanical in etiology
- Etiology: Peroneus brevis
- Chronic: subluxing tendon can splay or split over the sharp posterolateral edge of the fibula
- Acute: compression of the peroneus brevis tendon between the posterior fibula and peroneus longus tendon causes a split lesion during an inversion injury
- Both can lead to the so-called 'split lesion'
- Etiology: Peroneus Longus
- Acute: laceration of the tendon, avulsion of the tendon at or through the os peroneum, or dislocation at the lateral malleolus
Anatomy of the Lateral Compartment of the Leg and Peroneal Tendons
- Contains Peroneus Longus, Peroneus Brevis (sometimes referred to as Fibularis)
- Functions: Eversion, weak ankle plantarflexion, dynamic ankle stabilizer
- Both tendons cross the joint posteriorly to the lateral malleolus
- Tendon orientation at the level of the ankle is brevis anterioromedial to longus
- They share a common synovial sheath until they pass the fibula where they divide into separate sheaths
- Os peroneum
- Seen in about 20% of population[8]
- Ossified sesamoid bone at the level of the calcaneocuboid joint
- Peroneus Quartus
- Most commonly runs form the peroneus brevis to the retrotrochlear eminence of the calcaneus
- Associated with peroneus brevis tears, and subluxation
- Peroneal Tunnel
- Superior peroneal retinaculum
- Posterior fibula with a retromalleolar groove
- Calcaneofibular Ligament
Risk Factors
- Biomechanical/ Structural
- Hindfoot Varus
- Shallow or convex fibular groove
- Compression by the peroneus longus in dorsiflexion
- Hypertrophied peroneal tubercle and an enlarged retrotrochlear eminence
- Bony spur at the posterior lateral fibular groove
- Presence of peroneus quartus muscle in the peroneal sheath
- Orthopedic
- Systemic
- Pharmacology
- Fluoroquinolone Antibiotics
Differential Diagnosis
Differential Diagnosis Leg Pain
- Fractures & Dislocations
- Muscle and Tendon Injuries
- Neurological
- Vascular
- Other
- Pediatric Considerations
- Tibial Tubercle Avulsion Fracture
- Tibial Tuberosity Apophysitis
- Toddlers Fracture (Tibial Shaft Fracture)
Differential Diagnosis Ankle Pain
- Fractures & Dislocations
- Muscle and Tendon Injuries
- Ligament Injuries
- Bursopathies
- Nerve Injuries
- Arthropathies
- Pediatrics
- Fifth Metatarsal Apophysitis (Iselin's Disease)
- Calcaneal Apophysitis (Sever's Disease)
- Triplane Fracture
- Other
Clinical Features
History
- Patients typically report posterolateral hindfoot or ankle pain
- The tendon may look swollen or enlarged (more commonly in brevis than longus tears)[12]
- Patients may describe a snapping sensation
Physical Exam: Physical Exam Ankle
- Swelling proximal to or at lateral malleolus: brevis pathology
- Swelling at or distal to peroneal tubercle: longus pathology
- Pain with resisted eversion, ankle dorsiflexion
- Pain with passive inversion, ankle plantar flexion
- Subluxation/ crepitus of the peroneal tendon over posterior fibula can sometimes be palpated
- Strength may be diminished
- Presence of eversion does not exclude rupture or tear
- Rotate the ankle to see and feel if the tendons subluxate anteriorly over the lateral malleolus
Special Tests
- Peroneal Tunnel Compression Test: foot is dorsiflexed, everted with pressure applied to the retrofibular region of the peroneal tendons
- Plantarflex 1st Ray: loss or limitation of plantarflexion suggests dysfunction of peroneus longus
- Peroneal Tendon Dislocation Test: ask patient to plantarflex and evert, observe for subluxation or dislocation
Evaluation
Radiographs
- Standard Radiographs Ankle, Standard Radiographs Foot
- Standard views
- Axillary Heel View: can demonstrate the peroneal tubercle and the retromalleolar groove
- Os Peroneum
- Seen in 20% of the population
- visible on internal rotation oblique foot radiographs at the level of the calcaneocuboid joint
- Migration of the os peroneum proximal can suggest peroneal longus tendon disruption[13]
MRI
- Imaging modality of choice
- Findings of peroneal tendonitis/ tendonosis
- Peritendinous fluid
- Findings of peroneal subluxation/ dislocation
- Information on the status of the SPR
- Documenting the shape of the fibular groove
- Findings of peroneus longus tear
- Heterogeneity and/or discontinuity of the tendon
- Empty, fluid-filled tendon sheath
- Marrow edema along the lateral calcaneal wall
- Hypertrophied peroneal tubercle
- Diagnostic accuracy
- Magic Angle Effect
- Factitious appearance of heterogeneity, increased signal in a tendon when it intersects the main magnetic vector at an angle of 55°[16]
- Peroneal tendons are susceptible to this, especially at the tip of the lateral malleolus
Ultrasound
- When comparing diagnostic ultrasound to the gold standard of operative exploration[17][18]
- Sensitivity: 100%
- Specificity: 85-90%
- Diagnostic Accuracy: 90-94%
- Findings
- Peritendinous fluid is characteristic of tendonitis
Peroneal Tenography
- Involves the injection of radiopaque contrast medium into peroneal tendon sheaths to allow visualization of the tendon
- Infrequently used, suboptimal diagnostic technique which makes it a limited method
- Can co-administer local anesthetic and other medications
CT
- Useful to evaluate bony pathology
- Not generally indicated for peroneal tendon disease
Classification
- Based on pathology
- Tendinitis/ Tendinosis
- Tendon Tears/ Ruptures
- Tendon Dislocations/ Subluxation
Krause and Brodsky Classification for Tears
- Designed to help guide surgical decision making[19]
- Grade I are lesions that are less than 50% of cross-sectional area
- Intervention: tendon repair is recommended
- Grade II are lesion that are more than 50% of cross-sectional area
- Intervention: tenodesis is recommended
Eckert and Davis Classification for Superior Peroneal Retinaculum
- Classification for degree of SPR injury[20]
- Grade I: SPR elevated from fibula
- Grade II: Fibrocartilaginous ridge elevated from fibula with SPR
- Grade III: Cortical fragment avulsed with SPR
Management
Nonoperative
- Indications
- Vast majority of patients
- Eckert type I injuries
- Activity modification
- Medications
- Immobilization
- Tears: 4-8 weeks in a Tall Walking Boot or brace
- Tendinosis: Consider Tall Walking Boot for 4-6 weeks in refractory cases
- Physical Therapy
- Lateral Heel Wedge
- Corticosteroid Injection
- Should be performed under ultrasound guidance and can be considered for tendinosis/ tendonitis
Operative
- Indications
- Failure of conservative measures
- Acute subluxation/ dislocation
- Tear: Techniques
- Repair
- Tenodesis
- Reconstruction
- Allograft Reconstruction
- Tendonitis/ Tendinosis Techniques
- Synovectomy
- Excision of peroneus quartus muscle
- Peroneal tubercle osteotomy
- Subluxation/dislocation Techniques
- Primary repair of SPR
- Groove deepening procedures
- Bone block
- Tendon rerouting
- Reconstruction of SPR
Rehab and Return to Play
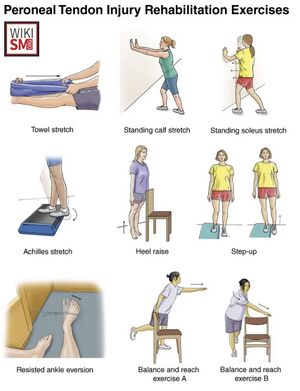
Rehabilitation
- Surgical
- Non-weightbearing 2-6 weeks
- Begin weight bearing in a cast or walking brace
- Median immobilization period is 6-8 weeks[21]
Return to Play/ Work
- Surgical
- Needs to be updated
- Non-surgical
- Typically within 1-2 weeks
- Recommend Lace Up Ankle Brace or Kinesiology Tape initially
- Can ween or discontinue as strength and function return to 90-100% of the unaffected ankle
Prognosis and Complications
Prognosis
- Tendinosis/ Tendonitis
- Majority of cases will resolve with conservative measures
Complications
- Surgical
- Most common: parasthesia of incision site from damage to branches of the Sural Nerve
- Healing issues
- Scarring, recurrent tears, degeneration
- Ankle Instability
See Also
Internal
External
References
- ↑ Monteggia, G: Instiuzini chirurgiche parte secondu. Milan, Italy: 336-341, 1803
- ↑ 35. Meyers, AW: Further evidences of attrition in the human body. Am. J. Anat. 34:241-267, 1924
- ↑ 24. Jones, E: Operative treatment of chronic dislocations of the peroneal tendons. JBJS 14 A: 574-576 , 1932
- ↑ 10. Burman, MS: Subcutaneous rupture of the tendon of the peroneal tendon. Ann Surg. 100: 368-372, 1934
- ↑ 5.0 5.1 Dombek MF, Lamm BM, Saltrick K, Mendicino RW, Catanzariti AR. Peroneal tendon tears: a retrospective review. J Foot Ankle Surg 2003;42:250-258.
- ↑ Sammarco, GJ, Diraimondo, CV. Chronic peroneus brevis tendon lesions. Foot Ankle Int. 1989;9(4):163–170.
- ↑ Krause, JO, Brodsky, JW. Peroneus brevis tendon tears: pathophysiology, surgical reconstruction, and clinical results. Foot Ankle Int. 1998;19(5):271–279.
- ↑ . Sobel, M; Pavlov, H; Geppert, MJ; Thompson, FM; DiCarlo, EF; Davis, WH: Painful os peroneum syndrome: a spectrum of conditions responsible for plantar lateral foot pain. Foot Ankle Int. 15:107-111, 199466
- ↑ Rosenberg, ZS; Feldman, F; Singson, RD; Price, GJ: Peroneal tendon injury associated with calcaneal fractures: CT findings. AJR Am. J. Roentgenol. 149:125-129, 1987
- ↑ Vainio, K: The rheumatoid foot. A clinical study with pathological and roentgenological comments. Ann. Chir. Gynaecol. Fenniae. 45:Suppl.1, 1-167, 1956
- ↑ . Truong, DT; Dussault, RG; Kaplan, PA: Fracture of the os peroneum and rupture of the peroneus longus tendon as a complication of diabetic neuropathy. Skeletal Radiol. 24(8):626-628, 1995
- ↑ 27. Molloy, R, Tisdel, C. Failed treatment of peroneal tendon injuries. Foot Ankle Clin. 2003;8(1):115–129.
- ↑ 51. Stockton, KG, Brodsky, JW. Peroneus longus tears associated with pathology of the os peroneum. Foot Ankle Int. 2014;35(4):346–352.
- ↑ Lamm, BM; Myers, DT; Dombek, M; Mendicino, RW; Catanzariti, AR; Saltrick K. Magnetic Resonance Imagings and surgical correlation of Peroneus Brevis Tears.J. Foot Ankle Surg. 43(1): 30-36, 2004
- ↑ Redfern, D; Myerson, M: The management of concomitant tears of the peroneus longus and brevis tendons. Foot Ankle Int. 25(10):695-707, 2004
- ↑ Gyftopoulos, S, Bencardino, JT. Normal variants and pitfalls in MR imaging of the ankle and foot. Magn Reson Imaging Clin N Am. 2010;18(4):691–705.
- ↑ Grant, TH, Kelikian, AS, Jereb, SE, McCarthy, RJ. Ultrasound diagnosis of peroneal tendon tears: a surgical correlation. J Bone Joint Surg Am. 2005;87(8):1788–1794.
- ↑ Waitches, GM; Rockett, M; Brage, M; Sudakoff, G: Ultrasonographic-surgical correlation of ankle tendon tears. J. Ultrasound Med. 17(4):249-256, 1998
- ↑ Krause, JO; Brodsky, JW: Peroneus brevis tendon tears: pathophysiology, surgical reconstruction and clinical results. Foot Ankle Int. 19(5):271-279, 1998.
- ↑ Eckert, WR; Davis, EA Jr: Acute rupture of the peroneal retinaculum. J Bone Joint Surg Am. 58(5): 670-672, 1976
- ↑ van Dijk, PA, Lubberts, B, Verheul, C, DiGiovanni, CW, Kerkhoffs, GMMJ. Rehabilitation after surgical treatment of peroneal tendon tears and ruptures. Knee Surg Sport Traumatol Arthrosc. 2016;24(4):1165–1174.
Created by:
John Kiel on 11 June 2019 01:47:14
Authors:
Last edited:
22 April 2026 15:45:27
Categories:

