Posterior Tibial Tendon Dysfunction
Other Names
- Tibialis Posterior Tendinopathy
- Posterior Tibial Tendon Dysfunction (PTTD)
- Posterior Tibialis Tendon Insufficiency
- Tibialis Posterior Tendon Rupture
- Tibialis Posterior Tendonitis
- Tibialis Posterior Dysfunction
- Peroneal Tendon Instability
Background
- This page refers to both acute and chronic injuries of the Tibialis Posterior tendon
- Generally, this refers to posterior tibial tendon dysfunction (PTTD)
- Other tendinopathies of the tibialis posterior are also discussed here
History
- Needs to be updated
Epidemiology
- Epidemiology is poorly described in the literature
- Typically unilateral, bilateral disease is uncommon[1]
- Prevalence
- Estimated to be between 3.3% and 10% of the population (need citation)
Introduction
- See: Tendinopathies (Main)'
Posterior Tibial Tendon Dysfunction (PTTD)
- Progressive, degenerative condition of the tibialis posterior tendon
- Typically occurs in obese, middle-aged women
- Results in progressive pes planus, hindfoot valgus and dysfunction of the posterior foot
- This can cause limitations in mobility, significant pain and weakness
Etiology
- Acute/Traumatic
- Inflammation of tendon can be seen after an acute injury such as ankle fracture, direct trauma to tendon[2]
- Tendinitis/ Tendonosis
- Repetitive microtrauma leading to tendinopathy is more common than an acute traumatic injury
- Tends to occur in hypovascular region along the medial malleolus
- Chronic
- Degeneration of tendon can be seen with overuse or chronic tendinopathies that are untreated
- Once the tendon becomes inflamed or torn, or loses function, the medial longitudinal arch of the foot begins to collapse
- The patient will develop relative internal rotation of tibia and talus[3]
- Eversion of subtalar joint, heel moves into valgus alignment, abduction of talonavicular joint
- Contracture of the Achilles tendon can occur with a lateral shift of the normal axis[4]
- Anatomic contributions may include
- Sharp turn behind the medial malleolus taken by the tibialis posterior
- The Flexor Retinaculum
- Abnormal anatomy of the talus
- Degenerative changes associated with osteoarthritis
- Pre-existing Pes Planus (as opposed to acquired pes planus from PTTD)
Associated Conditions
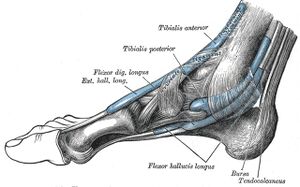
Anatomy of the Posterior Tibialis
- Originates in the Deep Posterior Compartment of the Leg
- Attaches along plantar surface of multiple tarsal, metatarsal bones
- Aids in plantarflexion, inversion and supports medial arch of foot
- Hypovascular area prone to degeneration is approx. 0.6 to 2.2 cm proximal to the medial malleolus[5]
Risk Factors
- General
- Recent increase or change in activity or training
- Morbid Obesity
- Older age
- Systemic
- Hypertension
- Diabetes Mellitus
- Seronegative Spondyloarthropathies
- Iatrogenic
- Oral Corticosteroids or Corticosteroid Injection[6]
- History of previous surgery
- Orthopedic/ Biomechanical
- Pes Planus
- Overpronation
- Other
- Foot and ankle trauma
Differential Diagnosis
Differential Diagnosis Ankle Pain
- Fractures & Dislocations
- Muscle and Tendon Injuries
- Ligament Injuries
- Bursopathies
- Nerve Injuries
- Arthropathies
- Pediatrics
- Fifth Metatarsal Apophysitis (Iselin's Disease)
- Calcaneal Apophysitis (Sever's Disease)
- Triplane Fracture
- Other
Clinical Features

History
- Typically insidious without an acute cause
- Pain most commonly located posterior to the medial malleolus, medial hind foot
- May have medial longitudinal arch pain
- Pain worse with activity, especially push off phase during gait
- Trouble walking on uneven surfaces, up or down stairs
- In more chronic patients, they may have hind foot pain
- Abnormal shoe wear pattern
Physical Exam: Physical Exam Foot And Ankle
- Tenderness with palpation of the tibialis posterior tendon, especially posterior to the medial malleolus
- Pain and/or weakness with resisted inversion and plantarflexion of the ankle
- Medial ankle pain with standing heel raise
- May have overpronated foot and/or planovalgus foot deformity
- Valgus hindfoot, equinus contracture may be present
Special Tests
- Too Many Toes Sign: Too many toes seen on affected limb from posterior evaluation
- Single Limb Heel Rise: Patient performs a single limb heel raise
- Posterior Tibial Length Test: test the length and function of tibialis posterior
Evaluation

Radiographs
- Standard Radiographs Ankle, Standard Radiographs Feet
- Should be weight bearing
- Findings
- May be normal early on
- Collapse of medial longitudinal arch
- Joint degeneration
- Increased talonavicular uncoverage
- Increased talo-first metatarsal angle (or Simmons angle)
MRI
- Findings
- Tendon changes (early)
- Degeneration (later)
Ultrasound
- Can evaluate
- Tendon size
- Degree of degeneration
- Presence of fluid
Classification

Johnson and Strom Classification
- I: Inflamed, intact tendon without clinical deformity[3]
- Able to perform single leg heel rise
- Mild tenosynovitis
- IIA: Ruptured or non-functional tendon with planovalgus deformity
- Arch collapse on a radiograph
- Unable to perform single-heel raise
- IIB: Ruptured or non-functional tendon with planovalgus deformity
- Arch collapse and talonavicular uncoverage (over 40%) on a radiograph
- Unable to perform single heel raise
- Flexible flatfoot deformity
- Characteristic forefoot abduction
- “too many toes” sign
- Flexible flatfoot deformity
- III: Advanced foot deformity with subtalar joint osteoarthritis
- Subtalar arthritis on a radiograph
- Unable to perform single heel raise
- Flatfoot deformity with rigid forefoot abduction, hindfoot valgus
- IV: Ankle joint involvement with tibio-talar degeneration
- Valgus deformity of talus in the ankle mortise visualized on AP radiograph of the ankle
- Talar tilt due to deltoid ligament compromise
- Subtalar arthritis on radiographs
- Unable to perform single heel raise,
- Flatfoot deformity with rigid forefoot abduction and hindfoot valgus
Management
Nonoperative
- Indications
- Most PTTD Stage I, some stage II
- Most forms of tendonitis or tendinosis
- Patients who are mostly sedentary or poor surgical candidate
- Activity modification
- Immobilization with Tall Walking Boot
- Duration 3-4 weeks (followed by PT)
- Orthotics including Shoe Inserts, Ankle Foot Orthosis
- Physical Therapy
- Emphasis on stretching Achilles tendon, strengthen tibialis posterior
- Eccentric exercises
- NSAIDS
Operative
- Indications
- Some PTTD stage II, most stage III/IV
- Failure of conservative management after 3-4 months
- Technique
- II: calcaneal osteotomy, posterior tibial tendon excision, flexor digitorum longus transfer, and achilles tendon lengthening
- III: triple arthrodesis (calcaneocuboid, talonavicular and subtalar joints)
- IV: Ankle arthrodesis
Rehab and Return to Play/Work
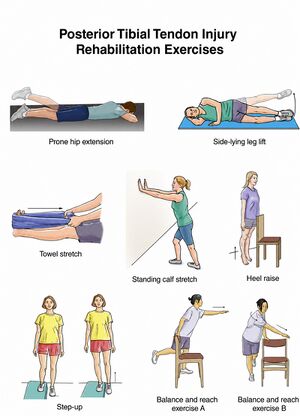
Rehabilitation
- Post surgical
- Non-weight bearing cast or splint for around 6 to 8 weeks
Return to Play/Work
- Needs to be updated
Complications
Prognosis
- PTTD
- Progressive degenerative process which will get worse if left untreated
- Stage I/II patients due well with orthosis and physical therapy, most patients returned to full strength at 4 months[9]
- Surgical outcomes in more severe cases produce less predictable results (need citation)
Complications
- Posterior tibialis tendon rupture
- Acquired Pes Planus
- Most common cause of acquired flat foot deformity in elderly patients
- Hindfoot Valgus
See Also
Internal
External
- Sports Medicine Review Ankle Pain: https://www.sportsmedreview.com/by-joint/ankle/
- Sports Medicine Review Foot Pain: https://www.sportsmedreview.com/by-joint/foot/
References
- ↑ Geideman WM, Johnson JE. Posterior tibial tendon dysfunction. J Orthop Sports Phys Ther. 2000;30:68–77
- ↑ Monto RR, Moorman CT, 3rd, Mallon WJ, Nunley JA., 3rd Rupture of the posterior tibial tendon associated with closed ankle fracture. Foot Ankle. 1991;11:400–3
- ↑ 3.0 3.1 Myerson M, Solomon G, Shereff M. Posterior tibial tendon dysfunction: Its association with seronegative inflammatory disease. Foot Ankle. 1989;9:219–25
- ↑ Mann RA. Acquired flatfoot in adults. Clin Orthop Relat Res. 1983:46–51.
- ↑ Manske MC, McKeon KE, Johnson JE, McCormick JJ, Klein SE. Arterial anatomy of the tibialis posterior tendon. Foot Ankle Int. 2015 Apr;36(4):436-43.
- ↑ Henceroth WD, 2nd, Deyerle WM. The acquired unilateral flatfoot in the adult: Some causative factors. Foot Ankle. 1982;2:304–8.
- ↑ Sung, Ki-Sun, and In-Sang Yu. "Acquired Adult Flatfoot: Pathophysiology, Diagnosis, and Nonoperative Treatment." Journal of Korean Foot & Ankle Society 18.3 (2014).
- ↑ 8.0 8.1 https://radiopaedia.org/cases/tibialis-posterior-tendon-dysfunction?lang=us
- ↑ Alvarez RG, Marini A, Schmitt C, Saltzman CL. Stage I and II posterior tibial tendon dysfunction treated by a structured nonoperative management protocol: an orthosis and exercise program. Foot Ankle Int. 2006 Jan;27(1):2-8.
Created by:
John Kiel on 26 June 2019 22:06:18
Authors:
Last edited:
9 June 2025 00:53:06
Categories:

