Sacroilliac Joint Pain
Other Names
- SI Joint Pain
- Sacroiliitis
- SIJ Pain
- Sacroiliac Joint Dysfunction
- Sacroiliac Pain
Background
- This page refers to back pain caused by pathology of the Sacroiliac Joint (SIJ)
History
- Needs to be updated
Epidemiology
- Prevalence
- 15-25% of axial low back pain arises from the SI Joint[4]
Introduction

General
- Patients typically present with deep pain radiating down posterior thigh and up to knee
- Worse/reproduced when sitting down, lying on ipsilateral side, climbing stairs
- Mechanism is often involves a combination of twisting/rotation and axial loading
- Between 40 and 50% of patients with injection-confirmed SIJ pain can identify a specific precipitating event
- Most frequently cited include motor vehicle collisions, falls, repetitive stress and pregnancy
- There is a paucity of literature on SIJ pain in athletes
- Asymmetric loading is likely a risk factor including kicking, swinging, throwing and single leg stance
Pathophysiology
- Thought to be caused by inflammation or injury to the joint capsule, ligaments or subachondral bone in the SI Joint[7]
- Pathologic changes can be broken down into intra-articular and extra-articular[8]
- Intra-articular: capsular or synovial disruption, capsular and ligamentous tension, abnormal joint mechanics, microfractures or macrofractures, chondromalacia,
- Extra-articular: hypomobility or hypermobility, extraneous compression or shearing forces soft tissue injury, and inflammation
Etiology
- Traumatic
- History of Pelvic Fracture
- Motor Vehicle Collision
- Torsion injuries from heavy lifting
- Atraumatic
- Osteoarthritis
- Spondyloarthropathies
- Pregnancy
- Scoliosis
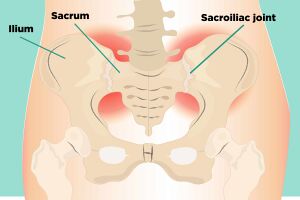
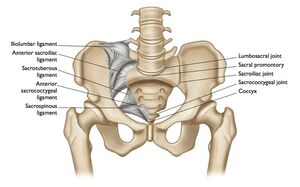
Anatomy of the Sacroiliac Joint
- Articulation of Sacrum and Ilium
- Diarthrodial Joint with fibrous capsule and synovial fluid
- Function: support the upper body, dampen the impact of ambulation, transfer weight from lower extremities to axial skeleton
Risk Factors
- Intrinsic[9]
- Extrinsic
- Gait or biomechanical dysfunction[12]
- Biomechanical abnormalities
- Spondyloarthropathies
- Other
- Sports
- Football
- Basketball
- Powerlifting
- Gymnastics
- Golf
- Cross country skiing[16]
- Rowing
- Use of eliptical, stair stepper
Differential Diagnosis
Differential Diagnosis Back Pain
- Fractures
- Neurological
- Musculoskeletal
- Autoimmune
- Infectious
- Pediatric
Clinical Features

History
- Pain patterns are highly variable, which makes clinical diagnosis challenging
- Although it can be traumatic, generally insidious from overuse
- Some patients endorse buttock pain extending into the posterolateral thigh[18]
- Slipman et al found patients reported buttock pain (94%), lumbar pain (72%), radiating into lower extremity (50%), pain below the knee (28%), and groin pain (14%)
- Worse with running, climbing stairs, standing from a seated position, lying on ipsilateral side
Physical Exam: Physical Exam Back
- May be tender over sacral sulcus
Special Tests
- FABER Test: Patient supine, affected limb is placed in figure 4 position (flexion, abduction, external rotation)
- Posterior Shear Test: Patient supine, stabilize SI joint, hip and knee flexed to 90° and posterior load applied
- Resisted Abduction Test: Patient supine, leg abducted about 30°, knee slightly flexed, asked to abduct against resistance
- Standing Flexion Test: Patient standing and flexes forward while examiner palpates PSIS and also on the S2 spinous process
- Stork Test: Patient stand on one leg while flexing the ipsilateral hip to 90° while examiner palpates PSIS and sacrum
- One Legged Hyperextension: Patient hyperextends backwards, examiner may help stabilize patient
- Sacroiliac Compression Test: Lateral decubitus on affected side, apply compression of SI joint
- Sacroiliac Distraction Test: Supine patient, apply force at bilateral ASIS
- Gaenslens Test: Supine, flex contralateral leg to chest, hang ipsilateral leg off the examination table
- Fortins Sign: Patient points to pain source with one finger, localizes to PSIS
- Cranial Shear Test: Patient prone, apply cranial directed force to sacrum
- Sacral Thrust Test: patient prone, apply anteriorly directed force to sacrum
- Active Straight Leg Raise Test: Patient holds straight leg a few inches off examination table
- Mennells Sign: with patient prone, extend hip and apply pressure to SI joint
- Shimpi Prone test: With patient prone, examiner palpates ASIS while patient extends hip
Evaluation
Diagnostic Sacroiliac Joint Injection
- Diagnostic gold standard
- History, exam and imaging are generally not enough to make diagnosis of SI joint pain
- Diagnostic confidence is 90%[21]
- Some variability to 'positive' test
- Most commonly accepted is at least 75% reduction if symptoms with injection[22]
- If less than 50%, consider other etiologies
- Reported success rates based on approach
- Injectant is typically anesthetic plus/minus corticosteroids
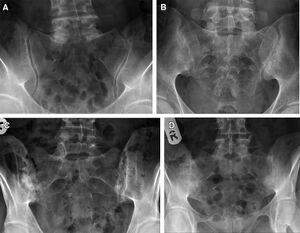
Radiographs
- Standard Radiographs Pelvis
- Of limited utility do to overlying osseous structures
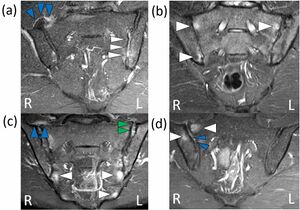
MRI
- Sensitivity >90%[26]
- Indicated if inflammatory condition is suspected
- Not useful in identifying non-inflammatory conditions
CT
- Elgafy et al: Using injection confirmed SI Joint Pain[27]
- Sensitivity 57.5%
- Specificity 69%
Radionuclide Imaging
- Sensitivity 13% - 46.1%[28]
- Specificity 89.5% - 100%
Classification
- Needs to be updated
Management
Nonoperative
- Indications
- First line therapy for nearly all cases
- Medications
- Topical and oral NSAIDS
- Acetaminophen
- Muscle Relaxants
- Consider Gabapentinoids
- Topical agents such as Menthol, Lidocaine
- Consider Duloxetine, Topiramate
- Activity Modification
- Physical Therapy
- Spinal Manipulation Therapy
- Includes manual therapy, osteopathic manual treatment, chiropractic adjustments
- Well designed studies fail to show benefit[31]
- Needs to be updated
- Prolotherapy
- Kim et al: Significant difference in symptoms at 15 minutes in prolotherapy arm vs steroid arm (control)[32]
- Platelet Rich Plasma (PRP)
- Mesenchymal Stem Cells
- According to the American Society of Interventional Pain Physicians (ASIPP) Guidelines, the literature is currently limited[35]
- Sacroiliac Joint Injection with corticosteroids
- Typically indicated when NSAIDS and PT have failed
- Performed with ultrasound or fluoroscopic guidance
- Benefit increases when combined with PT[36]
- Intra-articular injections generate more pain relief compared to peri-articular injections[37]
- Can also be used diagnostically (see evaluation)
- Extra-articular (EA): Appear to be superior to placebo[38]
- Intra-articular (IA): Appear to be superior to placebo[39]
- EA injections may be superior to IA according to Murakami et al[40]
- Neurolysis/ Radiofrequency Ablation
- Best candidates are those that have obtained relief from SI joint blocks
- Technique include heat (convential radiofrequency), bipolar, cold (cryoneurolysis), chemical (alcohol/phenol), pulsed, combined
- One retrospective study showed reduced opioid use, pain and disability relief[41]
- Consider Orthosis
- Shoe inserts for pes planus or pes cavus
- Heel Lift for leg length discrepancy
- Sacroiliac Brace if dysfunction is due to hypermobility
Operative
- Indications unclear
- Refractory to conservative measures? At least 6 months
- Must have had positive diagnostic injection
- In the setting of trauma
- Technique
- Open SIJ Fusion
- Minimally invasive SIJ Fusion
Rehab and Return to Play
Rehabilitation
- If present, correct maladaptive biomechanics[42]
- Most physical therapy protocols emphasize on core strengthening[43]
- Including correction of muscle imbalances, retraining of posture and proprioception
- In peri- and post-partum women, emphasis on strengthening the pelvic girdle
- Emphasis on improving range of motion of hip flexors, glutes, adductors
- Proposed program
- Closed, kinetic chain strength training to strengthen core, lumbo-pelvic musculature
- Progression to multiplanar strengthening exercises
- Consider gait analysis
- Techniques: direct manipulation, direct mobilization, indirect methods[44]
Rehab Exercise Program PDFs
- Sacroiliac Joint Pain Patient Education PDF
- Sacroiliac Joint Pain Exercises PDF
- SI Joint Stretches and Exercises PDF
- Sacroiliac Joint Home Exercise Program PDF
- Sacroiliac Joint Exercises PDF
Return to Play
- Prior to beginning RTP, ahlete should be[45]
- Relatively pain free, off medications
- Have no correctable biomechanical dysfunction
- Have successfully initiated rehabilitative program
- Achieved at least 75% of their baseline strength and flexibility
- If athlete has ankylosing spondylitis
- Screen for cardiac abnormalities
Prognosis and Complications
Prognosis
- Vanaclocha etal: study with up to 6 years follow up[46]
- Patients treated with conservative management had no long term improvement in pain, disability scores
- Increased use of opioids, poor long term work status
- Minimally invasive surgical techniques[47]
- Compared to open fusion: less tissue damage, blood loss, duration of hospitalization
- Better outcomes
- Operative complications occur in 21% of open, 18% of minimally invasive patients[48]
- Minimally invasive group had better pain scores at 12 and 24 months
Complications
- Chronic pain
- Inability to return to sport/ work
- Surgical complications[49]
- New-onset facet joint pain
- Trochanteric Bursitis
- Deep wound infections
- New onset low back or leg pain
- Superficial cellulitis
- Radiculopathy
- Avascular necrosis of the hip
- Piriformis Syndrome
- Implant penetration into the sacral neural foramen
- Peripheral Neuropathy
- Nondisplaced fracture
- Pulmonary Emboli/Deep Vein Thrombosis
See Also
Internal
External
References
- ↑ Depalma MJ, Ketchum JM, Trussell BS, Saullo TR, Slipman CW. Does the location of low back pain predict its source? PM R. 3(1), 33-39 (2011).
- ↑ Simopoulos TT, Manchikanti L, Singh V et al . A systematic evaluation of prevalence and diagnostic accuracy of sacroiliac joint interventions. Pain Physician 15(3), 305-344 (2012).
- ↑ Bernard TN, Kirkaldy-Willis WH. Recognizing specific characteristics of nonspecific low back pain. Clin Orthop 1987;217: 266 – 80.
- ↑ Cohen SP. Sacroiliac joint pain: A comprehensive review of anatomy, diagnosis and treatment. Anesth Analg. Published online 2005. doi:10.1213/01.ANE.0000180831.60169.EA
- ↑ Image courtesy of https://teachmeanatomy.info/, "The Sacroiliac Joint"
- ↑ Image courtesy of https://3dmusclelab.com/, "Exploring The Sacroiliac Joint
- ↑ Szadek KM, Hoogland PVJM, Zuurmond WWA, De Lange JJ, Perez RSGM. Possible nociceptive structures in the sacroiliac joint cartilage: An immunohistochemical study. Clin Anat. Published online 2010. doi:10.1002/ca.20908
- ↑ Cohen, S. P. (2005). Sacroiliac Joint Pain: A Comprehensive Review of Anatomy, Diagnosis, and Treatment. Anesthesia & Analgesia, 101(5), 1440–1453. doi:10.1213/01.ane.0000180831.60169.ea
- ↑ Cohen SP. Sacroiliac joint pain: a comprehensive review of anatomy, diagnosis, and treatment. Anesth. Analg. 101(5), 1440-1453 (2005).
- ↑ Schuit D, McPoil TG, Mulesa P. Incidence of sacroiliac joint malalignment in leg length discrepancies. J Am Podiatr Med Assoc 1989;79:380 –3.
- ↑ Schoenberger M, Hellmich K. Sacroiliac dislocation and scoliosis. Hippokrates 1964;35:476 –9.
- ↑ Herzog W, Conway PJ. Gait analysis of sacroiliac joint patients. J Manipulative Physiol Ther 1994;17:124 –7
- ↑ Marymont JV, Lynch MA, Henning CE. Exercise-related stress reaction of the sacroiliac joint: an unusual cause of low back pain in athletes. Am J Sports Med 1986;14:320 –3.
- ↑ Ostgaard HC, Andersson GB, Karlsson K. Prevalence of back pain in pregnancy. Spine 16(5), 549-552 (1991).
- ↑ Katz V, Schofferman J, Reynolds J. The sacroiliac joint: a potential cause of pain after lumbar fusion to the sacrum. J Spinal Disord Tech 2003;16:96 –9
- ↑ Butcher JD. Cross-country ski injuries. In: O’Connor F, Casa D, Davis B, et al. editors. ACSM’s Sports Medicine: A Comprehensive Review. 1st ed. Philadelphia (PA): Wolters Kluwer Lippincott Williams and Wilkins; 2013. p. 598.
- ↑ Bernstein, Robert M., and Harold Cozen. "Evaluation of back pain in children and adolescents." American family physician 76.11 (2007): 1669-1676.
- ↑ Fortin JD, Aprill CN, Ponthieux B, Pier J. Sacroiliac joint: pain referral maps upon applying a new injection/arthrography technique. Part II: Clinical evaluation. Spine 19(13), 1483-1489 (1994).
- ↑ Kok, Hong Kuan, et al. "Imaging the patient with sacroiliac pain." Canadian Association of Radiologists' Journal 67.1 (2016): 41-51.
- ↑ Braga, Marcio Vale, et al. "Prevalence of sacroiliitis and acute and structural changes on MRI in patients with psoriatic arthritis." Scientific Reports 10.1 (2020): 11580.
- ↑ Szadek KM, van der Wurff P, van Tulder MW, et al. Diagnostic validity of criteria for sacroiliac joint pain: a systematic review. J. Pain. 2009; 10:354–68.
- ↑ Rashbaum RF, Ohnmeiss DD, Lindley EM, et al. Sacroiliac joint pain and its treatment. Clin. Spine Surg. 2016; 29:42–8.
- ↑ D'Orazio F, Gregori LM, Gallucci M. Spine epidural and sacroiliac joints injections — when and how to perform. Eur. J. Radiol. 2014; 84:777–82.
- ↑ Chang WH, Lew HL, Chen CP. Ultrasound-guided sacroiliac joint injection technique. Am. J. of Phys. Med. Rehab. 2013; 92:278–9.
- ↑ D'Orazio F, Gregori LM, Gallucci M. Spine epidural and sacroiliac joints injections — when and how to perform. Eur. J. Radiol. 2014; 84:777–82.
- ↑ Puhakka KB, Jurik AG, Schiøttz-Christensen B et al . MRI abnormalities of sacroiliac joints in early spondylarthropathy: a 1-year follow-up study. Scand. J. Rheumatol. 33(5), 332-338 (2004).
- ↑ 50 Elgafy H, Semaan HB, Ebraheim NA, Coombs RJ. Computed tomography findings in patients with sacroiliac pain. Clin. Orthop. Relat. Res. 382, 112-118 (2001).
- ↑ Maigne JY, Boulahdour H, Chatellier G. Value of quantitative radionuclide bone scanning in the diagnosis of sacroiliac joint syndrome in 32 patients with low back pain. Eur. Spine J. 7(4), 328-331 (1998).
- ↑ Zelle BA, Gruen GS, Brown S, et al. Sacroiliac joint dysfunction: evaluation and management. Clin. J. Pain. 2005; 21:446–55.
- ↑ Kamali F, Zamanlou M, Ghanbari A, Alipour A, Bervis S. Comparison of manipulation and stabilization exercises in patients with sacroiliac joint dysfunction patients: A randomized clinical trial. J Bodyw Mov Ther. 2019;23(1):177-182. doi:10.1016/j.jbmt.2018.01.014
- ↑ Flynn T, Fritz J, Whitman J et al . A clinical prediction rule for classifying patients with low back pain who demonstrate short-term improvement with spinal manipulation. Spine 27(24), 2835-2843 (2002).
- ↑ Kim WM, Lee HG, Jeong CW, Kim CM, Yoon MH. A randomized controlled trial of intra-articular prolotherapy versus steroid injection for sacroiliac joint pain. J. Altern. Complement. Med. 16(12), 1285-1290 (2010).
- ↑ Singla V, Batra YK, Bharti N, Goni VG, Marwaha N. Steroid vs. Platelet-Rich Plasma in Ultrasound-Guided Sacroiliac Joint Injection for Chronic Low Back Pain. Pain Pract. 2017;17(6):782-791.
- ↑ Wallace P, Bezjian Wallace L, Tamura S, Prochnio K, Morgan K, Hemler D. Effectiveness of Ultrasound-Guided Platelet-Rich Plasma Injections in Relieving Sacroiliac Joint Dysfunction. Am J Phys Med Rehabil. 2020;99(8):689-693. doi:10.1097/PHM.0000000000001389
- ↑ Navani A, Manchikanti L, Albers SL, et al. Responsible, Safe, and Effective Use of Biologics in the Management of Low Back Pain: American Society of Interventional Pain Physicians (ASIPP) Guidelines.
- ↑ Schilling LS, Markman JD. Corticosteroids for Pain of Spinal Origin. Epidural and Intraarticular Administration. Rheum Dis Clin North Am. 2016;42(1):137-155. doi:10.1016/j.rdc.2015.08.003
- ↑ Althoff CE, Bollow M, Feist E, et al. CT-guided corticosteroid injection of the sacroiliac joints: quality assurance and standardized prospective evaluation of long-term effectiveness over six months. Clin Rheumatol. 2015;34(6):1079-1084. doi:10.1007/s10067-015-2937-7
- ↑ Luukkainen R, Nissilä M, Asikainen E et al . Periarticular corticosteroid treatment of the sacroiliac joint in patients with seronegative spondylarthropathy. Clin. Exp. Rheumatol. 17(1), 88-90 (1999).
- ↑ Maugars Y, Mathis C, Berthelot JM, Charlier C, Prost A. Assessment of the efficacy of sacroiliac corticosteroid injections in spondylarthropathies: a double-blind study. Br. J. Rheumatol. 35(8), 767-770 (1996).
- ↑ Murakami E, Tanaka Y, Aizawa T, Ishizuka M, Kokubun S. Effect of periarticular and intraarticular lidocaine injections for sacroiliac joint pain: prospective comparative study. J. Orthop. Sci. 12(3), 274-280 (2007).
- ↑ Tinnirello A. Reduction of opioid intake after cooled radiofrequency denervation for sacroiliac joint pain: a retrospective evaluation up to 1 year. Korean J Pain. 2020;33(2):183-191. doi:10.3344/kjp.2020.33.2.183
- ↑ Prather H, Hunt D. Conservative management of low back pain, part I. Sacroiliac joint pain. Dis. Mon. 50(12), 670-683 (2004).
- ↑ Mens JM, Snijders CJ, Stam HJ. Diagonal trunk muscle exercises in peripartum pelvic pain: a randomized clinical trial. Phys. Ther. 80(12), 1164-1173 (2000).
- ↑ Schmidt GL, Bhandutia AK, Altman DT. Management of sacroiliac joint pain. J Am Acad Orthop Surg. 2018;26(17):610-616. doi:10.5435/JAAOS-D-15-00063
- ↑ Peebles, Rebecca, and Christopher E. Jonas. "Sacroiliac joint dysfunction in the athlete: diagnosis and management." Current sports medicine reports 16.5 (2017): 336-342.
- ↑ Vanaclocha V, Herrera JM, Sáiz-Sapena N, Rivera-Paz M, Verdú-López F. Minimally invasive sacroiliac joint fusion, radiofrequency denervation, and conservative management for sacroiliac joint pain: 6-Year comparative case series. Neurosurgery. 2018;82(1):48-55. doi:10.1093/neuros/nyx185
- ↑ Smith AG, Capobianco R, Cher D, et al. Open versus minimally invasive sacroiliac joint fusion: a multi-center comparison of perioperative measures and clinical outcomes. Ann Surg Innov Res. 2013;7. doi:10.1186/1750-1164-7-14
- ↑ Martin CT, Haase L, Lender PA, Jr DWP. Minimally Invasive Sacroiliac Joint Fusion: The Current Evidence. Int J Spine Surg. 14:20-29. doi:10.14444/6072
- ↑ Zaidi HA, Montoure AJ, Dickman CA. Surgical and clinical efficacy of sacroiliac joint fusion: A systematic review of the literature. J Neurosurg Spine. 2015;23(1):59-66. doi:10.3171/2014.10.SPINE14516
Created by:
John Kiel on 17 June 2019 16:43:32
Authors:
Last edited:
3 March 2026 02:00:04
Categories:


