Herniated Disc
(Redirected from Degenerative Disc Disease)
Other Names
- Lumbar Disc Herniation (LDH)
- Thoracic Disc Herniation
- Disc Disease
- Disc Herniation
- Herniated Nucleus Pulposus (HNP)
- Degenerative Disc Disease
- LDH with radiculopathy
- Lumbar Intervertebral Disc Herniation (IDH)
- Slipped disc
- Prolapsed disc
- Intervertebral disc herniation
- Ruptured disc
- Disc prolapse
Background
- This page refers to both acute and chronic pathology of the Intervertebral Disc
History
- Needs to be updated
Epidemiology
- As much as 80% of people develop lower back pain during their lifetime[1]
- Nearly all involve L4/5 or L5/S1 levels (need citation)
- Peak incidence 4th, 5th decade of life (need citation)
- Males more common than females by a ratio of 3:1 (need citation)
Introduction

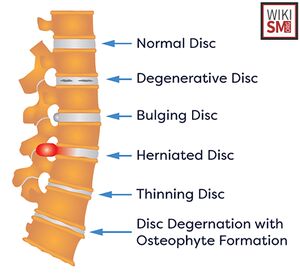
General
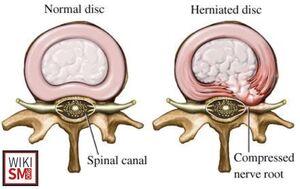
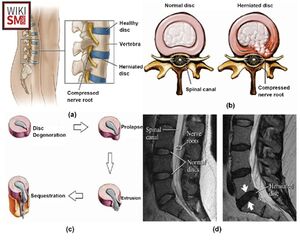
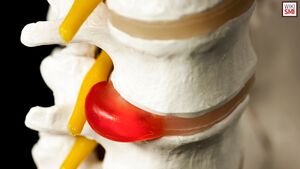
- Characterized by displacement of intervertebral disc material beyond the normal margins of the disc space
- Herniated discs are extremely common on imaging in asymptomatic individuals
- The diagnosis is made clinically and confirmed on MRI
- Approximately 87% of patients experiencing decreased pain within 3 months without surgery[6]
Etiology
- Dehydration is known to contribute to degenerative disc disease[7]
- Axial Overloading
- Not all cases are degenerative, insidious disc disease
- Static overloading, as opposed to physiologic and dynamic overloading, put the disc at risk for posterior herniation[8]
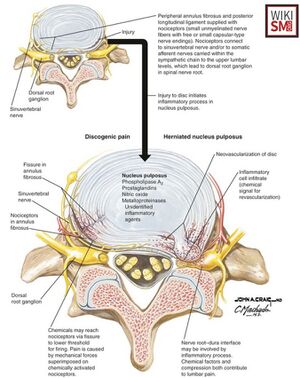
- Inflammation
- The role of inflammatory signaling in producing nerve pain in LDH has been well-established
- Propionibacterium acnes
- Gram-positive, facultative anaerobic, fastidious bacterium, which may play a central role in LDH[9]
- Normally associated with superficial skin infections, most notably ace
- 2001 study: 53% of patients had gram positive anaeorbes, of which 84% were P. acnes[10]
- Aghazadeh et al: P. acnes DNA correlates to vertebral edema on preoperative MRI[11]
- In rabit models, Chen et al demonstrated the bacteria induced disc degeneration[12]
- Other studies have failed to reproduce these findings and more research is needed
- Acidosis
- Cuesta et al: pH of degenerative discs is ~1.0 less than that of healthy discs[13]
Terminology
- Herniated disc (herniated nucleus pulposus)
- Displacement of intervertebral disc material beyond the normal margins of the disc space
- Involves less than 25% of the disc circumference
- May include elements of the nucleus pulposus, annulus fibrosus, or both
- Annular tear (annular fissure)
- Disruption or crack in the annulus fibrosus
- Degenerative disc disease (DDD)
- An aberrant, cell-mediated response to progressive structural failure
- Characterized by structural defects combined with accelerated signs of aging
- Spinal stenosis: Narrowing of the spinal canal
Anatomy of the Intervertebral Disc
- Consists of inner nucleus pulposus (NP), outer annulus fibrosis (AF)
- NP: comprised of collagen, proteoglycans, acts to resist axial compression of the spine[14]
- AF: Composed of type I collagen, supports and maintains the NP
- Tearing of AF leads to protrusion of NP
- Posterior Longitudinal Ligament (PLL): Helps stabilize discs posteriorly
- Functions
- Forms a fibrocartilaginous joint between the bodies of adjacent vertebrae
- Binds the vertebral column together
- Provides shock absorption
- Prevents friction between vertebrae
Primary Associated Conditions
- Spinal Stenosis
- Lumbar Radiculopathy/ Sciatica
- #1 cause of radicular back pain in patients under age of 60[15]
- Low Back Pain
Secondary Associated Conditions
- Cauda Equina Syndrome
- Estimated to occur between 1% - 10% of patients with herniated discs[16]
- Degenerative Disc Disease
- Progressive degeneration with loss of hydration of the nucleus pulposus precedes HNP development
- Facet Joint Arthropathy
- Spondylolisthesis
- Can occur with or contribute to nerve root compression in the setting of disk herniation[17]
- Chronic radiculopathy
- Persistent nerve root symptoms may occur after disk herniation, with or without surgical intervention
Risk Factors
Genetic
- Familial aggregation and twin studies that genetic predisposition may account for a significant portion of risk[6]
- Specific genes[18]
- Collagen genes (particularly collagen IX)
- Aggrecan
- Vitamin D receptor
- Matrix metalloproteinase genes
Occupational
- Heavy lifting and lumbar load (OR = 2.1)[19]
- Whole-body vibration, particularly from motor vehicle driving
- Torsional stress and repetitive bending or twisting
- Night shift work (OR = 23.01)
Lifestyle factors
- Tobacco Use Disorder[20]
- Higher body mass index
- Lack of regular physical exercise (OR = 0.5 for protective effect)
- Chronic inflammation
Additional Factors
- Older Age
- Male sex
- Younger age at presentation
- History of Trauma
- Congestive Heart failure
Protective
- Sleeping on a hard bed (OR = 0.4)
Differential Diagnosis
Differential Diagnosis Back Pain
- Fractures
- Neurological
- Musculoskeletal
- Autoimmune
- Infectious
- Pediatric
Clinical Features
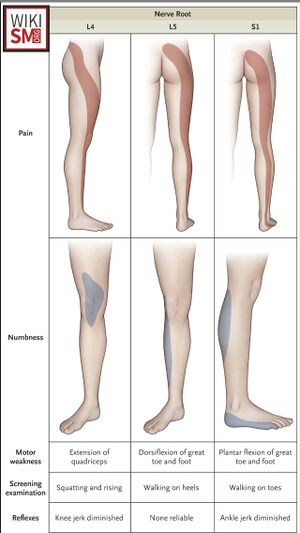
History
- Clasically presents as lower back pain
- Patients may endorse radicular features, sensory abnormalities and weakness
- Often radiating below the knee in a dermatomal distribution[21]
- Symptoms may be worse with straining, coughing, sneezing[22]
- May be worse with sitting, improved with standing
- There may be a history of other back problems
Physical Exam: Physical Exam Back
- Affected dermatome varies based on level of herniation
- Findings tested based on level of radiculopathy
- L3: Hip adduction weakness
- L4: Knee extension weakness, decreased patellar DTR
- L5: weakened ankle dorsiflexion, inversion, EHL and hip abduction, heel walking
- S1: Weakned plantarflexion, decreased achilles DTR, toe walking
Special Tests
- Straight Leg Test (SLRT): Elevation of leg while supine or seated recreates radicular pain
- Sensitivity: 80%, specificity: 40%[6]
- Contralateral SLRT: Recreates symptoms by raising contralateral leg
- Sensitivity 28%, specificity 90%[23]
- Lesegue sign: SLRT worse with forced ankle dorsiflexion
- Bowstring sign: During SLRT, apply pressure to tibial nerve in popliteal fossa
- Kernigs Sign: pain reproduced with neck flexion, hip flexion, and leg extension
Evaluation
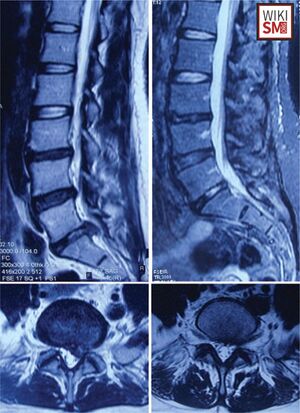
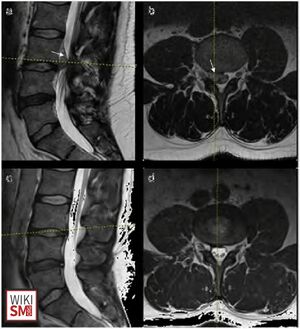
Clinical Diagnosis
- Initial screening with a positive straight leg test + 3 out of 4 of the following symptoms is sufficient for clinical diagnosis[26]
- Dermatomal pain, sensory deficits, reflex deficits, and/or motor weakness
- Imaging is not initially recommended for typical cases of herniated disc with radicular features
- Most guidelines recommend imaging only after 4 to 6 weeks of conservative treatment
- Early Imaging indicated for:
- Progressive or severe neurologic deficits
- Multiple nerve root involvement
- Red flags suggesting tumor, infection, or cauda equina syndrome
Radiographs
- First line imaging
- Findings in the setting of Herniated Disc
- Scoliosis (compensatory)
- Narrowed intervertebral disc space/ loss of disc height
- Traction osteophytes
- Loss of lordosis
- Degenerative spondylosis
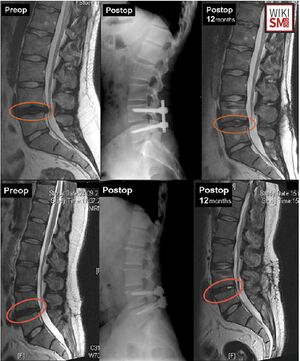
MRI
- Gold standard to confirm lumbar disc herniation, typically without contrast
- Diagnostic accuracy of 85-97%[27]
- Findings
- Increased T2-weighted signal from the posterior 10% of the disc diameter[28]
- Diffusion tensor imaging (DTI) can be used to detect microstructural changes in the nerve root
- High rate of abnormal findings in asymptomatic individuals
- Indications for obtaining MRI
- Pain lasting >6-12 weeks not responding to normal conservative therapy
- Presence of red flags
Modic Changes
- Represent pathologic changes to the vertebral body
- Type 1: vascular developments in the vertebral body including inflammation and edema
- correlate significantly with degree of degenerative disc disease
- Type 2: fatty replacement of the vertebral bone marrow
- Type 3: fractures or changes of the trabecular bone of the vertebrae
CT
- With myelography, diagnostically equivalent to MRI for lumbar disc herniation[29]
- Useful in patients who can not receive MRI
Electromyography
- Usually unnecessary but may help when symptoms or imaging findings are ambiguous
- Can reveal denervation patterns corresponding to specific nerve roots
Classification
Location Based Classification
- Central prolapse
- Associated with back pain only, cauda equina syndrome
- Posterolateral (paracentral)
- Represents >90% of cases due to weak PLL
- Affects descending or lower nerve root
- Foraminal (far lateral, extraforaminal)
- Less common, affecting 5-10% of cases
- Affects exiting or upper nerve root
- Axillary
- Can affect both upper and lower nerve root
Anatomic Classification
- Protrusion: eccentric bulging, intact annulus
- Extrusion: disc material herniates through annulus, remains continuous with disc space
- Sequestered fragment: disc material herniates through annulus, no longer continuous with disc space
Management
Nonoperative
- Indications
- Treatment of choice for the majority of patients
- Initial approach
- Very brief period of rest following by increasing activity as tolerated
- Patient education, NSAIDs, and exercise-based physical therapy for at least 4-6 weeks
- Bed rest does not accelerate recovery and should be avoided
- Patient education
- Patients should be informed of the favorable natural history
- Many improve within 6 weeks, with 36% reporting improvement at 2 weeks
- Medications
- NSAIDS
- Muscle Relaxants
- Consider Oral Corticosteroids
- Physical Therapy
Physical Therapy Modalities
- Spinal Traction
- One small study showed improvement in 28 day outcomes, however no control arm[33]
- Spinal Manipulation Therapy
- Consider chiropractor, massage therapy
- McKenzie Method
- Neural Mobilization
Procedural
- Corticosteroid Injection (CSI)
- Widely varied success rates from 20% to 95%[34]
- Thought to be due be more beneficial in acutely herniated discs, where a true inflammatory response is occurring.
- Provide short term improvement in radicular pain, sensory symptoms
- Likely do not reduce rate of surgical intervention, provide any functional benefit[35]
- Disc herniation <6.23 mm more likely to do well with CSI
- Platelet Rich Plasma (PRP)
- Several studies have reported improvement in clinical scores 1 month post PRP injection[36]
Interventions with conflicting or no evidence
- Traction (though one trial showed some benefit when added to medication and electrotherapy)
- Laser
- Ultrasound
- Electrotherapy
Operative
- Indications
- Consider: patients with pain persisting beyond 6-12 weeks who have congruent symptoms, examination findings, and MRI results
- Severe or progressive neurologic deficits
- Cauda Equina Syndrome
- Technique
- Microdiscectomy: laminotomy, discectomy
- Percutaneous lumbar foraminoplasty
- Far lateral microdiscectomy
- Open Discectomy
Rehab and Return to Play
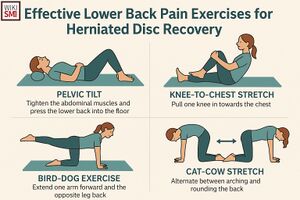
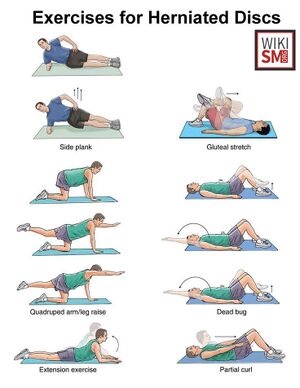
Rehabilitation
- Core components[37]
- Directional preference and centralization exercises (McKenzie method) should be utilized
- Trunk coordination, strengthening, and endurance exercises
- Strengthening exercises are recommended for nearly all patients
- Typical progression might include[38]
- Week 1: spinal manipulation followed by spinal range-of-motion exercises performed 10 repetitions, 3-4 times daily
- Week 2-3: Review of range-of-motion exercises and introduction of trunk-strengthening exercises targeting lumbar spine stabilizing muscles
- Weeks 3-6+: Exercise review and progression with continued focus on functional restoration
Rehab Programs/PDF
- Herniated Disc Rehabilitation PDF
- Herniated Disc Physical Therapy PDF
- Exercises for Herniated Disc PDF
- Slipped Disc Rehabilitation PDF
Return to Play
- General
- Individualized, function-based rehabilitation
- Addresses anatomical, physiological, functional, and psychological components of the injury
- Requires continuous evaluation of risk tolerance based on diagnosis and progress
- Timeline
- Most athletes can begin gradual return to sport after 3 months,[39]
- 48.4% typically recommend return to high levels of activity after 3 months
- In young athletes undergoing microdiscectomy, 71% returned to play at an average of 4.5 months postoperatively,
- Post-operative
- Athletes with herniated lumbar disks should rest 6 to 12 weeks following surgical treatment, while those with spinal fusion should wait 1 year to return to activity[40]
- High risk sports require special consideration
- Surgeons often recommend avoiding—sometimes permanently
- weightlifting (35.7%, rugby (21.4%), horseback riding (17.9%), and martial arts (14.3%)
Prognosis and Complications
Prognosis
- General
- Gugliotta et al: equivalent medium- and long-term outcomes for conservative and surgical treatment of LDH[41]
- Other studies have demonstrated improved 1- and 2-year outcomes in the surgical treated group when compared to conservatively managed patients
- Conservative
- 90% of patients will improve at 3 months with non-operative care (need citation)
- 81% of those with initial paresis recovered without surgery after 1 year, though sensory deficits may be more persistent (50% recovery at 1 year
- Herniated disc is reabsorbed over time and decreases in size
- Disc herniation >6.31 mm likely to benefit from surgical intervention
- Predictors of good surgical outcome
- Factors that do not affect surgical outcome
- Motor deficit
- Vertebral level or side of herniation
- Gender
- Presence of type I modic changes
Complications
- Cauda Equina Syndrome (CES)
- Rare, devastating
- Risk factors for dveloping CES: diabetes, acute onset of symptoms, L3-L4 involvement, sequestrated discs (fully separated NP from AF), superiorly migrated discs, posterior herniation, primary canal stenosis, and greater canal compromise[47]
- Dural Tear
- Rate of 1-17%
- Increases hospitilization cost, wound dehiscience, post op infection, worsening function, nerve injury[48]
- Recurrent herniation risk factors[49]
- Pre-operative disc height index
- Trauma
- Older age
- Smoking
- Disc protrusion
- Disc sequestration
- Longer duration of sick leave
- Workers’ compensation
- Greater preoperative symptom severity
- Diabetes Mellitus
- Discitis
- Vascular injury (vena cava or aorta)
See Also
Internal
External
- Sports Medicine Review Back Pain: https://www.sportsmedreview.com/by-joint/back/
References
- ↑ Andersson GB. Epidemiological features of chronic low-back pain. Lancet. 1999;354(9178):581–585.
- ↑ Camargo, Perea, and Rodrigo Dennis. "Electro-mechanical characterization of piezo-metallic cellular solids for spine implants." Masters Abstracts International. Vol. 48. No. 05. 2010.
- ↑ Ratish, Singh, et al. "Percutaneous endoscopic lumbar spine surgery for lumbar disc herniation and lumbar spine stenosis: Emphasizing on clinical outcomes of transforaminal technique." Surgical Science 9.02 (2018): 63.
- ↑ Image courtesy of aneskey.com
- ↑ Khan, Aysha N., et al. "Inflammatory biomarkers of low back pain and disc degeneration: a review." Annals of the new york academy of sciences 1410.1 (2017): 68-84.
- ↑ 6.0 6.1 6.2 6.3 Deyo, Richard A., and Sohail K. Mirza. "Herniated lumbar intervertebral disk." New England Journal of Medicine 374.18 (2016): 1763-1772.
- ↑ Brayda-Bruno M, Tibiletti M, Ito K, et al. Advances in the diagnosis of degenerated lumbar discs and their possible clinical application. Eur Spine J. 2014;23(SUPPL. 3):315–323.
- ↑ Paul CPL, de Graaf M, Bisschop A, et al. Static axial overloading primes lumbar caprine intervertebral discs for posterior herniation. PLoS One. 2017:1–23
- ↑ Albert HB, Sorensen JS, Christensen BS, Manniche C. Antibiotic treatment in patients with chronic low back pain and vertebral bone edema (modic type 1 changes): a double-blind randomized clinical controlled trial of efficacy. Eur Spine J. 2013;22(4):697–707.
- ↑ Stirling A, Worthington T, Rafiq M, Lambert PA, Elliott TSJ. Association between sciatica and Propionibacterium acnes. Lancet. 2001;357(9273):2024–2025. doi: 10.1016/S0140-6736(00)05109-6.
- ↑ Aghazadeh J, Salehpour F, Ziaeii E, Javanshir N. Modic changes in the adjacent vertebrae due to disc material infection with Propionibacterium acnes in patients with lumbar disc herniation. Eur Spine J. 2016;
- ↑ Chen Z, Zheng Y, Yuan Y, et al. Modic changes and disc degeneration caused by inoculation of Propionibacterium acnes inside intervertebral discs of rabbits: a pilot study. Biomed Res Int. 2016;2016.
- ↑ Cuesta A, Del Valle ME, García-Suárez O, et al. Acid-sensing ion channels in healthy and degenerated human intervertebral disc. Connect Tissue Res. 2014;55(3):197–204.
- ↑ Kadow T, Sowa G, Vo N, Kang JD. Molecular basis of intervertebral disc degeneration and herniations: what are the important translational questions? Clin Orthop Relat Res. 2015;473(6):1903–1912.
- ↑ Knezevic, Nebojsa Nick, et al. "Treatment of chronic low back pain–new approaches on the horizon." Journal of pain research (2017): 1111-1123.
- ↑ Shapiro S. Cauda equina syndrome secondary to lumbar disc herniation. Neurosurg 1993; 32: 743–747.
- ↑ Earwood, J. Scott, Nancy A. Doles, and Raedeen S. Russell. "Acute Low Back Pain: Diagnosis and Management." American family physician 112.5 (2025): 526-536C.
- ↑ Ala-Kokko, Leena. "Genetic risk factors for lumbar disc disease." Annals of medicine 34.1 (2002): 42-47.
- ↑ Zhang, Yin-gang, et al. "Risk factors for lumbar intervertebral disc herniation in Chinese population: a case-control study." Spine 34.25 (2009): E918-E922.
- ↑ Li, Zhonghai, et al. "Clinical characteristics and risk factors of recurrent lumbar disk herniation: a retrospective analysis of three hundred twenty-one cases." Spine 43.21 (2018): 1463-1469.
- ↑ Zhang, Andrew S., et al. "Lumbar disc herniation: diagnosis and management." The American journal of medicine 136.7 (2023): 645-651.
- ↑ Vroomen P, de Krom M, Wilmink J, Kester A, Knottnerus J. Diagnostic value of history and physical examination in patients suspected of lumbosacral nerve root compression. J Neurol Neurosurg Psychiatry. 2002;72(5):630–634.
- ↑ Ropper, Allan H., and Ross D. Zafonte. "Sciatica." New England Journal of Medicine 372.13 (2015): 1240-1248.
- ↑ Qi, Lei, et al. "The clinical application of “jetting suture” technique in annular repair under microendoscopic discectomy: a prospective single-cohort observational study." Medicine 95.31 (2016): e4503.
- ↑ Ilozue, Tagbo, et al. "Symptomatic Disc Herniations: A Review to Understand Pathophysiology and Prediction of Outcomes."
- ↑ Petersen T, Laslett M, Juhl C. Clinical classification in low back pain: best-evidence diagnostic rules based on systematic reviews. BMC Musculoskelet Disord. 2017;18(1):188.
- ↑ Kim KY, Kim YT, Lee CS, Kang JS, Kim YJ. Magnetic resonance imaging in the evaluation of the lumbar herniated intervertebral disc. Int Orthop. 1993;17(4):241–244.
- ↑ Messner A, Stelzeneder D, Trattnig S, et al. Does T2 mapping of the posterior annulus fibrosus indicate the presence of lumbar intervertebral disc herniation? A 3. 0 Tesla magnetic resonance study. Eur Spine J. 2017;26:877–883.
- ↑ Janssen ME, Bertrand SL, Joe C, Levine MI. Lumbar herniated disk disease: comparison of MRI, myelography, and post-myelographic CT scan with surgical findings. Orthopedics. 1994;17(2):121–127
- ↑ Egemen, E., et al. "Perspective of lumbar segmental instability for surgical evaluation of lumbar disc herniation." J Spine 6.354 (2017): 2.
- ↑ Jewell DV, Riddle DL. Interventions that increase or decrease the likelihood of a meaningful improvement in physical health in patients with sciatica. Phys Ther. 2005;85(11):1139–1150.
- ↑ Thackeray A, Fritz J, Lurie J, Zhao W, Weinstein J. Nonsurgical treatment choices by individuals with lumbar intervertebral disc herniation in the United States: associations with long-term outcomes. Am J Phys Med Rehabil. 2016:1–8.
- ↑ Isner-Horobeti M-E, Dufour SP, Schaeffer M, et al. High-force versus low-force lumbar traction in acute lumbar sciatica due to disc herniation: a preliminary randomized trial. J Manip Physiol Ther. 2016;39(9):645–654.
- ↑ Kepes ER, Duncalf D. Treatment of backache with spinal injections of local anesthetics, spinal and systemic steroids. A review. Pain. 1985;22(1):33–47.
- ↑ Carette S, Leclaire R, Marcoux S, et al. Epidural corticosteroid injections for sciatica due to herniated nucleus pulposus. N Engl J Med. 1997;336:1634–1640.
- ↑ Levi D, Horn S, Tyszko S, Levin J, Hecht-Leavitt C, Walko E. Intradiscal platelet-rich plasma injection for chronic discogenic low back pain: preliminary results from a prospective trial. Pain Med. 2015:pnv053.
- ↑ Hegmann, Kurt T., et al. "Non-invasive and minimally invasive management of low back disorders." Journal of occupational and environmental medicine 62.3 (2020): e111-e138.
- ↑ Fritz, Julie M., et al. "Early physical therapy vs usual care in patients with recent-onset low back pain: a randomized clinical trial." Jama 314.14 (2015): 1459-1467.
- ↑ Bäcker, Henrik C., et al. "Return to sports following discectomy: does a consensus exist?." European Spine Journal 33.1 (2024): 111-117.
- ↑ Eck JC, Riley LH., III Return to play after lumbar spine conditions and surgeries. Clin Sports Med. 2004;23:367-379
- ↑ Gugliotta M, Costa BR, Dabis E, et al. Surgical versus conservative treatment for lumbar disc herniation: a prospective cohort study. BMJ Open 2016:1–7. 10.1136/bmjopen-2016-012938.
- ↑ Weinstein JN, Tosteson TD, Lurie JD, et al. Surgical vs nonoperative treatment for lumbar disk herniation. JAMA. 2006;296(20):2441.
- ↑ Osterman H, Seitsalo S, Karppinen J, Malmivaara A. Effectiveness of microdiscectomy for lumbar disc herniation. Spine (Phila Pa 1976) 2006;31(21):2409–2414.
- ↑ Oba H, Takahashi J, Tsutsumimoto T, et al. Predictors of improvement in low back pain after lumbar decompression surgery: prospective study of 140 patients. J Orthop Sci. 2017:6–11.
- ↑ Tschugg A, Lener S, Hartmann S, et al. Preoperative sport improves the outcome of lumbar disc surgery: a prospective monocentric cohort study. Neurosurg Rev. 2017; 10.1007/s10143-017-0811-6.
- ↑ Wilson CA, Roffey DM, Chow D, Alkherayf F, Wai EK. A systematic review of preoperative predictors for postoperative clinical outcomes following lumbar discectomy. Spine J. 2016;16(11):1413–1422.
- ↑ Krishnan V, Rajasekaran S, Aiyer SN. Clinical and radiological factors related to the presence of motor deficit in lumbar disc prolapse: a prospective analysis of 70 consecutive cases with neurological deficit. Eur Spine J. 2017.
- ↑ Puvanesarajah V, Hassanzadeh H. The true cost of a dural tear. Spine (Phila Pa 1976) 2017;42(10):770–776.
- ↑ Hegarty D, Shorten G. Multivariate prognostic modeling of persistent pain following lumbar discectomy. Pain Physician. 2012;15(5):421.
Created by:
John Kiel on 17 June 2019 15:27:30
Authors:
Last edited:
21 January 2026 12:14:37
Categories:

