Scaphoid Fracture
Other Names
- Scaphoid non union
- Occult scaphoid fracture
- Carpal Scaphoid Fracture
- Wrist Scaphoid Fracture
- Carpal Navicular Fracture
- Navicular Fracture (hand)
- Scaphoid Waist Fracture
- Proximal Pole Scaphoid Fracture
Background
- This page refers to fractures of the Scaphoid bone
History
- The scaphoid fracture was first formally described in 1905 by the French surgeon and radiologist Destot[1]
- Early literature referred to the scaphoid as the “navicular bone of the hand,” reflecting its boat-like shape and historical confusion with the tarsal navicular bone.[2]
- In the 20th century, recognition of the scaphoid’s tenuous retrograde blood supply led to early understanding of complications such as nonunion and avascular necrosis[3]
- A major advancement in management occurred in 1984 when Herbert and Fisher introduced the **headless compression (Herbert) screw**, revolutionizing surgical fixation and improving union rates.[4]
Epidemiology
- Scaphoid is most commonly fractured carpal bone[5]
- 10% of all hand fractures and 60% of all carpal fractures[5]
- 15% of wrist fractures (need citation)
- Incidence is highest in young, active males aged 15–30 years due to higher exposure to trauma.[6]
- These injuries are relatively uncommon in children and older adults due to differences in bone structure and injury patterns.[7]
Introduction



General
- Scaphoid fractures are a common cause traumatic wrist pain and are the most common carpal bone fracture
- Retrograde blood supply makes scaphoid particular susceptible to avascular necrosis and nonunion
- Diagnosis is made radiographically, with a high incidence of occult fractures and missed diagnosis
- Treatment is often surgical although select cases can be treated conservatively
Location
- 65% occur in the waist[5]
- 25% proximal 1/3rd, which has an increased risk of AVN
- 10% distal 1/3rd, which has a higher rate of union
Etiology
- Traumatic injury which typically involves fall on outstretched hand[10]
- Wrist is hyper-extended with radial deviation
- Axial load / sports trauma
- Rare stress fractures[6]
Anatomy of the Scaphoid
- Boat-shaped carpal bone on radial side of the wrist[11]
- Spans proximal & distal carpal rows
- Articulates with radius, lunate, capitate, trapezium, trapezoid
- The retrograde blood supply (distal → proximal) makes it particularly vulnerable[12]
- Proximal pole has poorest vascularity (↑ AVN risk)
- Function is to aid in movement of the wrist, forms the radial border of the carpal tunnel
Associated Injuries
- Scapholunate Ligament Injury (most common)[13]
- Perilunate Dislocation / carpal instability[14]
- Distal Radius Fracture (combined injury)[5]
- TFCC Injury[15]
- Acute Carpal Tunnel Syndrome[12]
Risk Factors
Patient Factors
- Male sex, age 15–30
- High activity / contact sports
- Tobacco Use Disorder
Mechanism / Injury Factors
- FOOSH with wrist hyperextension[16]
- High-energy trauma (sports, MVC, falls)
Fracture-Specific Factors (Complication Risk)
- Proximal pole fracture (↑ AVN)
- Displacement or comminution
- Delayed diagnosis or treatment
Anatomic / Vascular Factors
- Retrograde blood supply
- Limited vascularity of proximal pole
Differential Diagnosis
Carpal Bone Fractures
- Scaphoid Fracture
- Lunate Fracture
- Triquetrum Fracture
- Pisiform Fracture
- Trapezium Fracture
- Trapezoid Fracture
- Capitate Fracture
- Hamate Fracture
Differential Diagnosis Wrist Pain
- Fractures
- Dislocations
- Wrist Dislocation (Radiocarpal and/or Ulnocarpal)
- Carpometacarpal Joint Dislocation
- Distal Radioulnar Joint Dislocation
- Lunate Dislocation
- Perilunate Dislocation
- Instability & Degenerative
- Tendinopathies & Ligaments
- Neuropathies
- Pediatric Considerations
- Distal Radial Epiphysitis (Gymnast's Wrist)
- Torus Fracture
- Arthropathies
- Cartilage
- Vascular
- Other
Clinical Features

History
- Patients will some history of trauma, typically a FOOSH
- Will complain of wrist pain or thumb pain, worse with movement or activity
- The pain may be vague, hard to localize
- Worse with gripping, pinching
- Range of motion is decreased
- Initially, patient may be able to continue activity
Physical Exam: Physical Exam Wrist
- Mild swelling over radial wrist
- Deformity is typically absent
- These 3 exam findings reported to be 100% sensitive, 74% specific for scaphoid fracture in first 24 hours following injury[18]
- Scaphoid compression test
- Snuffbox tenderness
- Palpation of the volar scaphoid tubercle
- Pain with resisted pronation
Special Tests
- Scaphoid Shift Test: apply pressure to scaphoid with ulnar and radial deviation
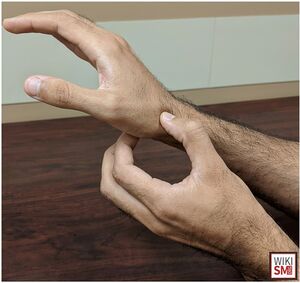
- Clamp Sign: Patient will form a clamp with the opposite thumb and index finger over scaphoid
- Scaphoid Compression Test: Apply an axial load down the thumb to compress the scaphoid
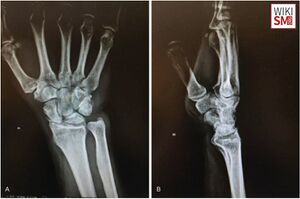
Evaluation



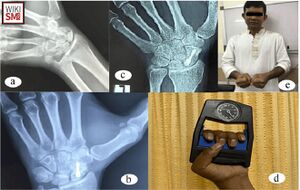
Radiographs
- Standard Radiographs Wrist
- Scaphoid View: PA view in ulnar deviation
MRI
- Most sensitive for occult fractures
- Pooled sensitivity of 88% and specificity of 100% in meta-analysis[19]
- Can evaluate for other soft tissue pathology
- Cost-effectiveness analysis: MRI is superior to empiric cast immobilization, reducing both costs and morbidity[21]
CT
- Diagnostic accuracy
- Pooled sensitivity of 72%, specificity of 99%[22]
- Useful for assessing
- Fracture fragments
- Extent of collapse
- Pre-operative planning
Bone Scan
- Falling out of favor, remains an option
- Highest sensitivity among imaging modalities at 99%, lower specificity 86%[19]
Ultrasound
- For radiographically occult scaphoid fractures, pooled sensitivity of 85.6% and specificity of 83.3%[23]
- Advantages: rapid, non-invasive, point-of-care modality without radiation exposure
- Dynamic ultrasound can also evaluate for fracture stability
- However, operator dependendent and not widely used for scaphoid imaging
Classification
Herbert and Fisher's Classification of Scaphoid Fractures
- Type A: Stable acute fractures
- A1: Tubercle fracture
- A2: Incomplete waist fracture
- Type B: Unstable acute fractures
- B1: Distal oblique fractures
- B2: Complete or displaced waist fracture
- B3: Proximal pole fracture
- B4: Transscaphoid perilunate dislocation fracture
- B5: Comminuted fracture
- Type C: Delayed union
- Type D: Established nonunion
- D1: Fibrous union
- D2: Pseudoarthrosis
Management
Nonoperative
- Indications
- Stable, nondisplaced (majority)
- Normal radiographs with high index of suspicion
- Minimally displaced scaphoid waist and distal pole fractures
- Incomplete fractures
- Confirmed stable fractures without displacement
- Suspected Fracture
- In patients with normal radiographs, but a high degree of clinical suspicion,
- Patients should be placed in a thumb spica splint or thumb spica brace
- Repeat radiographs in roughly 1-2 weeks
- Confirmed Fracture
- Management decisions should be made in consultation with an orthopedic surgeon
- The majority of scaphoid fractures are nondisplaced or minimally displaced
- Can be treated with immobilization for 6-10 weeks in a thumb spica cast
- One study showed Below-elbow casting without thumb immobilization improved outcomes[5]
Operative
- Indications[25]
- Displaced fractures (>2 mm displacement or step-off)
- Proximal pole fractures (prone to nonunion due to tenuous blood supply)
- Unstable fracture patterns
- Patient preference for faster return to activity (particularly athletes)
- Confirmed nonunion after conservative treatment
- Technique
- Standard Single Screw Fixation
- Dual Screw Fixation
- Plate Fixation
Rehab and Return to Play
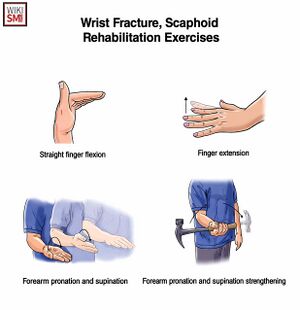
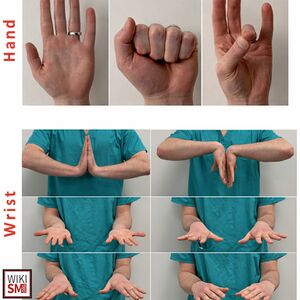
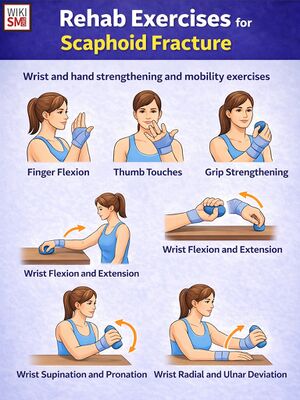
General Rehab Principles
- Healing first: confirm union (prefer CT) before advancing
- Early protection: strict immobilization initially
- Imaging-guided: don’t rely on exam alone
- Protect loading: avoid early grip, impact, weight-bearing
- Maintain motion: keep shoulder, elbow, fingers moving
- ROM before strength: restore motion prior to resistance
- Criteria-based progression: healing + pain-free + functional ROM
- Control swelling/stiffness: elevation, compression, tendon glides
- Gradual strengthening: progress to functional/sport tasks
- Individualize care: fracture type, location, athlete demands
- Watch complications: nonunion, AVN, persistent pain
- Return to activity: only after union + full painless function
Phase 1: Protection & Early Mobilization[26]
- Nonoperative
- Immobilization: 6–10 weeks (below-elbow cast ± thumb)
- Thumb not required for nondisplaced waist/distal pole fractures
- Maintain: shoulder, elbow ROM; finger motion
- Progression: CT at ~6 weeks with ≥50% trabecular bridging
- Operative
- Immobilization: 0–2 weeks (variable)
- Post-op: immediate mobilization → short splinting (surgeon dependent)
- Maintain: early finger motion; guided wrist motion
- Progression: wound healing, pain control, surgeon clearance
Phase 2: Active ROM & Gentle Strengthening[27]
- Timeline: After cast removal (non-op) or per surgeon protocol (op)
- Goals
- Restore wrist ROM (flex/ext, radial/ulnar deviation)
- Restore forearm rotation (pronation/supination)
- Improve grip strength
- Reduce edema/stiffness
- Exercises
- Active wrist ROM (pain-free)
- Forearm rotation
- Gentle grip (putty/ball)
- Tendon gliding (fingers/thumb)
- Edema control (elevation/compression)
- Restrictions
- No heavy lifting or impact
- Avoid forceful grip or weight-bearing
- Progress by pain tolerance
- Duration: ~2–4 weeks
Phase 3: Strengthening & Functional Return
- Timeline
- Non-op: ~8–12 weeks
- Operative: ~6–10 weeks
- Prerequisites
- CT: ≥50% bridging (prefer full union)
- Minimal/no pain with ADLs
- ≥70% ROM vs contralateral side
- Goals
- Full wrist ROM
- Restore strength (wrist + grip)
- Return to ADLs
- Sport-specific progression
- Exercises
- Resistance training (wrist curls, extension, deviation)
- Progressive grip strengthening
- Proprioception/stability drills
- Functional/task-specific training
- Plyometrics (athletes)
- Duration: ~4–6 weeks
Scaphoid Fracture Rehab PDFs
- Scaphoid fracture rehab PDF
- Scaphoid wrist fracture rehab exercises PDF
- Scaphoid fracture physical therapy PDF
- Scaphoid fracture patient handout PDF
Return to play criteria

- Athletes should meet ALL of the following before unrestricted return
- Radiographic healing: CT confirmation of at least 50% trabecular bridging (complete union preferred for contact sports)
- Pain-free activity: No pain with sport-specific movements or loading
- Range of motion: At least 90% of contralateral wrist in all planes
- Strength: Grip strength at least 85-90% of contralateral side
- Functional testing: Successful completion of sport-specific drills without pain or apprehension
- Psychological readiness: Athlete confidence in returning to full participation
Playing Cast Option
- Indication: in-season athletes with stable, nondisplaced mid-third fractures
- Playing cast may allow immediate or early return (average 4.3 weeks)[28]
- Comparable union rates to those who delay return
- This option requires:
- Confirmed stable fracture pattern
- Appropriate sport (typically non-contact or limited contact)
- Custom-fitted protective cast
- Close monitoring for displacement or nonunion
- Shared decision-making with athlete regarding risks
Prognosis and Complications
Prognosis
- Overall
- Nonoperative
- >90% of union in scaphoid fractures with <1 mm displacement (need citation)
- Fracture Location and Healing
- Distal pole fractures: Best prognosis, highest union rates
- Waist fractures: Good prognosis with appropriate treatment; 10-15% fail to heal with casting alone
- Proximal pole fractures: Poorest prognosis due to tenuous blood supply; higher rates of nonunion and avascular necrosis (AVN)
- Displaced fractures[30]
- Displaced fractures (>1-2 mm) have significantly worse outcomes
- 55% incidence of nonunion and 50% rate of AVN if not anatomically reduced
Complications
- Avascular Necrosis
- From disruption of the scaphoid's fragile blood supply, which enters primarily from the distal pole
- Proximal pole fractures are particularly prone to AVN
- Non-union[31]
- Most significant complication
- Occurs in 10-15% of conservatively treated fractures and up to 10% after surgical treatment
- Risk factors include displacement, instability, delayed diagnosis, smoking, inadequate treatment, AVN
- Scaphoid Nonunion Advanced Collapse
- Untreated nonunion almost inevitably leads to degenerative wrist arthritis, typically within 5 years
- Malunion[32]
- Malunion with "humpback deformity" (flexion deformity of the scaphoid) can occur
- Leading to altered carpal mechanics and predisposing to degenerative changes
See Also
Internal
- Forearm Pain (Main)
- Wrist Pain (Main)
- Hand Pain (Main)
- Hand and Wrist Anatomy (Main)
- Physical Exam Wrist
External
References
- ↑ Rhemrev SJ, et al. Current methods of diagnosis and treatment of scaphoid fractures. 2011.
- ↑ Gray’s Anatomy; historical terminology review.
- ↑ Rhemrev SJ, et al. 2011.
- ↑ Herbert TJ, Fisher WE. The Herbert screw. 1984.
- ↑ 5.0 5.1 5.2 5.3 5.4 Buijze, Geert A., and Jesse B. Jupiter. "Acute Scaphoid Fractures: Guidelines for Diagnosis and Treatment." Journal of the American Academy of Orthopaedic Surgeons, vol. 19, no. 6, 2011, pp. 354–365.
- ↑ 6.0 6.1 Duckworth, A. D., et al. "The Epidemiology of Fractures of the Scaphoid." Journal of Bone and Joint Surgery, vol. 94-B, no. 10, 2012, pp. 1305–1310.
- ↑ Cooney, William P. "Scaphoid Fractures: Current Treatments and Techniques." Instructional Course Lectures, vol. 52, 2003.
- ↑ Case courtesy of Hani M. Al Salam, Radiopaedia.org, rID: 13037
- ↑ Hackney, Lauren A., and Seth D. Dodds. "Assessment of scaphoid fracture healing." Current reviews in musculoskeletal medicine 4 (2011): 16-22.
- ↑ Fowler, J. R., and J. P. Hughes. "Scaphoid Fractures." Clinical Sports Medicine, vol. 34, no. 1, 2015, pp. 37–50.
- ↑ Standring, Susan, ed. Gray’s Anatomy: The Anatomical Basis of Clinical Practice. 41st ed., Elsevier, 2016.
- ↑ 12.0 12.1 Gelberman, Richard H., and Daniel J. Menon. "The Vascularity of the Scaphoid Bone." Journal of Hand Surgery, vol. 5, no. 5, 1980, pp. 508–513.
- ↑ Fowler, J. R., and J. P. Hughes. "Scaphoid Fractures." Clinical Sports Medicine, vol. 34, no. 1, 2015, pp. 37–50.
- ↑ Herzberg, Guillaume. "Perilunate and Axial Carpal Dislocations and Fracture-Dislocations." Journal of Hand Surgery, vol. 33, no. 9, 2008, pp. 1659–1668.
- ↑ Palmer, A. K. "Triangular Fibrocartilage Complex Lesions: A Classification." Journal of Hand Surgery, vol. 14, no. 4, 1989, pp. 594–606.
- ↑ Fowler, J. R., and J. P. Hughes. "Scaphoid Fractures." Clinical Sports Medicine, vol. 34, no. 1, 2015, pp. 37–50.
- ↑ Coventry, Laura, et al. "Which clinical features best predict occult scaphoid fractures? A systematic review of diagnostic test accuracy studies." Emergency Medicine Journal (2023).
- ↑ Parvizi J, Wayman J, Kelly P, Moran CG. Combining the clinical signs improves diagnosis of scaphoid fractures. A prospective study with follow-up. J Hand Surg Br. 1998 Jun; 23(3):324-7
- ↑ 19.0 19.1 19.2 Mallee, Wouter H., et al. "Computed tomography versus magnetic resonance imaging versus bone scintigraphy for clinically suspected scaphoid fractures in patients with negative plain radiographs." Cochrane Database of Systematic Reviews 6 (2015).
- ↑ Daniels, Anne M., et al. "What is the diagnostic performance of conventional Radiographs and clinical reassessment compared with HR-pQCT scaphoid fracture diagnosis?." Clinical Orthopaedics and Related Research® 481.1 (2023): 97-104.
- ↑ Karl, John W., Eric Swart, and Robert J. Strauch. "Diagnosis of occult scaphoid fractures: a cost-effectiveness analysis." JBJS 97.22 (2015): 1860-1868.
- ↑ Gemme, Seth, and Robert Tubbs. "What physical examination findings and diagnostic imaging modalities are most useful in the diagnosis of scaphoid fractures?." Annals of Emergency Medicine 65.3 (2015): 308-309.
- ↑ Kwee, Robert M., and Thomas C. Kwee. "Ultrasound for diagnosing radiographically occult scaphoid fracture." Skeletal radiology 47.9 (2018): 1205-1212.
- ↑ Mohiuddin, Md, et al. "The outcome of scaphoid fracture nonunion managed by 1, 2 intercompartmental supraretinacular artery (1, 2 ICSRA) vascularized bone graft." Cureus 15.10 (2023).
- ↑ 25.0 25.1 25.2 Dias, Joseph J., et al. "Surgery versus cast immobilisation for adults with a bicortical fracture of the scaphoid waist (SWIFFT): a pragmatic, multicentre, open-label, randomised superiority trial." The Lancet 396.10248 (2020): 390-401.
- ↑ Dunleavy, Mark L., Nicholas Pilla, and Michael Darowish. "Treatment Options, Return to Play, and Functional Performance after Operatively and Non-operatively Managed Acute Scaphoid Fractures." Current Reviews in Musculoskeletal Medicine 18.1 (2025): 17-25.
- ↑ Hughes, Thomas B. "Acute scaphoid waist fracture in the athlete." Clinics in sports medicine 39.2 (2020): 339-351.
- ↑ Rettig, Arthur C., Erich J. Weidenbener, and Robert Gloyeske. "Alternative management of midthird scaphoid fractures in the athlete." The American journal of sports medicine 22.5 (1994): 711-714.
- ↑ Odella, Simona, et al. "Locking dorsal plate in four-bone arthrodesis in SLAC and SNAC 3 wrist." Joints 6.01 (2018): 037-041.
- ↑ Szabo, Robert M., and DAVID MANSKE. "Displaced fractures of the scaphoid." Clinical Orthopaedics & Related Research 230 (1988): 30-38.
- ↑ Kawamura, Kenji, and Kevin C. Chung. "Treatment of scaphoid fractures and nonunions." The Journal of hand surgery 33.6 (2008): 988-997.
- ↑ Gray, Robert RL, et al. "Scaphoid fracture and nonunion: new directions." Journal of Hand Surgery (European Volume) 48.2_suppl (2023): 4S-10S.

