Tarsal Tunnel Syndrome
Other Names
- Entrapment neuropathy of the posterior tibial nerve
- Tarsal Tunnel Syndrome (TTS)
- Posterior tibial neuralgia
Background
- This page describes entrapment of the Posterior Tibial Nerve (PTN) as it courses through the Tarsal Tunnel[1]
History
- First clinical description in 1918 by Von Malaise (need citation)
- Named by Keck and Lam in 1962 in two separate reports[2][3]
Epidemiology
- Relatively rare condition; epidemiology is not well described in the literature
Introduction


General
- Entrapment neuropathy of the PTN as it courses through the flexor retinaculum on the medial side of the ankle
- Rare disorder which causes motor and sensory deficits on the plantar aspect of the foot
- Diagnosis and management remain challenging to clinicians
Etiology
- Intrinsic
- Osteophytes from Ankle Arthritis
- Hypertrophic retinaculum
- Tendonopathy
- Space-occupying lesions such as enlarged veins, ganglia, lipoma, tumour and neuroma
- Haemorrhage secondary to trauma can lead to scarring, fibrosis
- Tarsalcalcaneal Coalition[8]
- Extrinsic
- Direct trauma
- Constrictive foot wear
- Hind foot varus or valgus
- Generalized lower limb edema (pregnancy, venous congestion)
- Systemic inflammatory arthropathies
- Diabetes Mellitus
- Post surgical scarring
- Mixed
- Can be due to more than one intrinsic or extrinsic cause
- Idiopathic
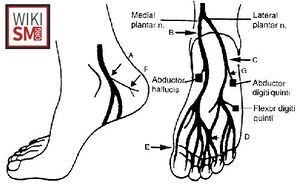
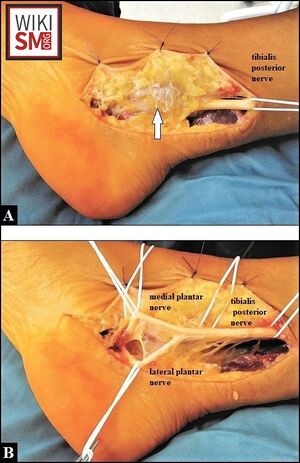
Anatomy of the Posterior Tibial Nerve
- Bifurcates into Medial Plantar Nerve, Lateral Plantar Nerve at the level of tarsal tunnel
- About 5% of patients bifurcate proximal to tarsal tunnel[9]
- Both the medial and lateral plantar nerves supply autonomic, sensory and motor fibres to the plantar foot[10]
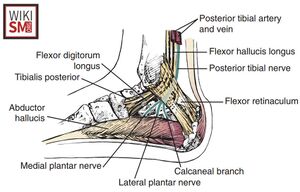
Anatomy of the Tarsal Tunnel
- Fibro-osseous tunnel beneath the flexor retinaculum, behind and inferior to the medial malleolus
- Floor: medial wall of the talus, calcaneus and the medial wall of the distal tibia
- Contents from medial to lateral:
- Tibialis Posterior Tendon
- Flexor Digitorum Longus Tendon
- Posterior Tibial Artery and vein
- Posterior Tibial Nerve
- Flexor Hallucis Longus tendon
Risk Factors
- Female > Male[11]
Differential Diagnosis
Differential Diagnosis Ankle Pain
- Fractures & Dislocations
- Muscle and Tendon Injuries
- Ligament Injuries
- Bursopathies
- Nerve Injuries
- Arthropathies
- Pediatrics
- Fifth Metatarsal Apophysitis (Iselin's Disease)
- Calcaneal Apophysitis (Sever's Disease)
- Triplane Fracture
- Other
Clinical Features

History
- Predominant symptom is pain directly over tarsal tunnel, behind medial mal radiating into the heel and plantar foot
- Paraesthesia, dysesthesia and hyperaesthesia along the medial ankle radiating into the sole, heel or digits [13]
- Burning, numbness, or tingling in the foot
- Worsens with standing and walking
- Night symptoms may be reported
- Improve with rest, elevation
- Note the dorsum of the foot should be asymptomatic
- Symptoms are rarely bilateral
Physical Exam: Physical Exam Ankle
- Tenderness on deep palpation of the tarsal tunnel
- Valleix Phenomenon: pain radiating proximally to the tarsal tunnel may be present
- Recommended to test two point discrimination on plantar surface[13]
Special Tests
- Tinel Test: Performed at medial malleolus may reproduce smptoms
- Dorsiflexion Eversion Test: Dorsiflex the ankle and toes with eversion can reproduce symptoms
- Triple Compression Stress Test: Ankle plantarflexed, inverted with direct pressure over tibial nerve
- Plantarflexion Inversion Test: place in maximal plantarflexion and inversion for 10 to 15 seconds
- Tarsal Tunnel Compression Test:
Evaluation
Radiology
- Standard Radiographs Ankle
- Often normal but looking for structural abnormalities
- Potential findings
- Hind foot varus/valgus
- Tarsal Coalitions
- Osteophytes
- Evidence of previous trauma
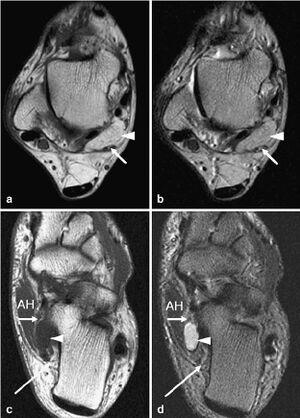
MRI
- General
Ultrasound
- May provide evidence of direct nerve compression
- Hypoechoic and never enlargement proximally to entrapment [17]
- Numkarunarunrote found it may provide evidence of nerve compression by demonstrating nerve enlargement, changes in echogenicity[18]
- Therimadasamy et al. found patients averaged a cross-sectional area of 0.17 cm2 on the pathological side vs. 0.10 cm2 on the unaffected side[19]
- Lee et al found mean cross-sectional area of 24 mm2 in patients with diabetic tibial nerve pathology vs. 12 mm2 in people without a neuropathy[20]
- Can be used to evaluate for[21]
- Ganglia
- Varicose veins
- Lipomas
- Tenosynovitis
- Talocalcaneal coalition
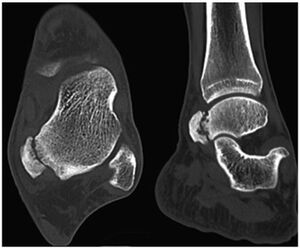
CT
- Can be considered if osseous abnormalities found in plain xray
EMG/NCS
- General
- Adjunct study that should be taken in context with history and exam
- Can not be used in isolation to make the diagnosis
- Evaluate motor and sensory function
- Sensitivity of EMG is 90% [22]
- Useful to distinguish patients with TTS and more proximal lesions
Classification
- Not applicable
Management
Nonoperative
- Indications
- Vast majority of cases are nonoperative initially
- However treatment should be directed at the specific cause
- Overall, the literature is weak regarding management of TTS
- NSAIDS
- Activity modification
- Physical Therapy
- Consider taping, bracing
- Stretching and strengthening of the calf, tibialis anterior and posterior, peroneal and short toe-flexor muscles
- Orthotics
- Orthotic shoes may decrease pressure over the nerve[24]
- Also consider night splint, removal boot walker
- Custom orthoses to support the medial and lateral longitudinal arches of the affected foot
- Procedures
- Aspiration of ganglia may provide temporary benefit
- Corticosteroid Injection if intra- or perineural edema
Operative
- Indications
- Failure of conservative management
- Definitive indications of entrapment
- Technique
- Tarsal tunnel release [25]
- Cryosurgery
Rehab and Return to Play
Rehabilitation
- Needs to be updated
Return to Play/ Work
- Needs to be updated
Complications and Prognosis
Prognosis
- Surgical release
- Predictors of good surgical outcome[28]
- Short history of foot pain
- Presence of a ganglion
- No history of trauma or sprain
- Light working duties
- Delay in decompression more than 10 months[27]
- Predictors of poor relief from surgery[29]
- Incorrect initial diagnosis
- Incomplete surgical release of the tarsal tunnel
- Adhesive neuritis following initial decompression measures
- Intraneural damage/disruption associated with direct neural trauma or systemic disease
- Presence of a space-occupying lesion or double crush syndrome
- Cryosurgery
- May be an effective alternative to standard surgical interventions[30]
Complications
- Chronic pain
- Sensory dysfunction
- Complex Regional Pain Syndrome
- Recurrence of symptoms
- Incomplete surgical release
- Postoperative scar formation at the surgical site[31]
See Also
Internal
External
- Sports Medicine Review Ankle Pain: https://www.sportsmedreview.com/by-joint/ankle/
- Sports Medicine Review Foot Pain: https://www.sportsmedreview.com/by-joint/foot/
References
- ↑ Luis Beltran, J. B. (2010). Entrapment Neuropathies III: Lower Limb. Seminars in Musculoskeletal Radiology, 501-511
- ↑ Keck C. The tarsal-tunnel syndrome. J Bone Joint Surg Am. 1962;44:180-2.
- ↑ Lam, S. J. S. "A tarsal-tunnel syndrome." The Lancet 280.7270 (1962): 1354-1355.
- ↑ McSweeney, Simon C., and Matthew Cichero. "Tarsal tunnel syndrome—a narrative literature review." The Foot 25.4 (2015): 244-250.
- ↑ Williams, Nicole, et al. "Tarsal tunnel syndrome in the mucopolysaccharidoses: A case series and literature review." JIMD reports 46.1 (2019): 16-22.
- ↑ Oh, Shin J. "Neuropathies of the foot." Clinical neurophysiology 118.5 (2007): 954-980.
- ↑ Kim, Jahyung, and Jaeho Cho. "Tarsal Tunnel Syndrome: A Narrative Review." The Nerve 10.1 (2024): 1-6.
- ↑ Lee, M. F., et al. "Tarsal tunnel syndrome caused by talocalcaneal coalition." Clinical imaging 26.2 (2002): 140-143.
- ↑ Havel PE, Ebraheim NA, Clark SE. Tibial branching in the tarsal tunnel. Foot Ankle 1988;9:117–9.
- ↑ 10.0 10.1 Reade BM, Longo DC, Keller MC. Tarsal tunnel syndrome. Clin Podiatr Med Surg 2001;18(3):395–408.
- ↑ Lau, John TC, and Tim R. Daniels. "Tarsal tunnel syndrome: a review of the literature." Foot & ankle international 20.3 (1999): 201-209.
- ↑ M Kinoshita, R. O. (2001). The Dorsiflexion-Eversion Test for Diagnosis of Tarsal Tunnel Syndrome. The Journal of Bone and Joint Surgery, 1835-1839
- ↑ 13.0 13.1 John Lau, T. D. (1999). Tarsal Tunnel Syndrome: A Review of the Literature. Foot & Ankle International, 201-209
- ↑ Sweed, Tamer Ahmed, Seyed Asghar Ali, and Surabhi Choudhary. "Tarsal tunnel syndrome secondary to an unreported ossicle of the talus: a case report." The Journal of Foot and Ankle Surgery 55.1 (2016): 173-175.
- ↑ Kim, Sungjun, et al. "Role of magnetic resonance imaging in entrapment and compressive neuropathy—what, where, and how to see the peripheral nerves on the musculoskeletal magnetic resonance image: part 2. Upper extremity." European radiology 17 (2007): 509-522.
- ↑ Frey, Carol, and Roger Kerr. "Magnetic resonance imaging and the evaluation of tarsal tunnel syndrome." Foot & ankle 14.3 (1993): 159-164.
- ↑ Jon Jacobson, T. W. (2016). Sonography of Common Peripheral Nerve Disorders With Clinical Correlation. The American Institute of Ultrasound in Medicine , 683-693.
- ↑ Numkarunarunrote, Numphung, et al. "Retinacula of the foot and ankle: MRI with anatomic correlation in cadavers." American Journal of Roentgenology 188.4 (2007): W348-W354.
- ↑ Therimadasamy, A., et al. "Combination of ultrasound and nerve conduction studies in the diagnosis of tarsal tunnel syndrome." Neurology India 59.2 (2011): 296.
- ↑ Lee, Doohi, and Damien M. Dauphinée. "Morphological and functional changes in the diabetic peripheral nerve: using diagnostic ultrasound and neurosensory testing to select candidates for nerve decompression." Journal of the American Podiatric Medical Association 95.5 (2005): 433-437.
- ↑ Nagaoka M, Matsuzaki H. Ultrasonography in tarsal tunnel syndrome. J Ultrasound Med 2005;24:1035–40.
- ↑ Troy Watson, R. A. (2002). Distal Tarsal Tunnel Release With Partial Plantar Fasciotomy for Chronic Heel Pain: An Outcome Analysis. Foot & Ankle International.
- ↑ Schmidt, Ingo. "Ledderhose’s Disease-What do We Know and What do We not know."
- ↑ Gessini L, Jandolo B, Pietrangeli A. The anterior tarsal syndrome. J Bone Joint Surg 1984;66A:786–7.
- ↑ Eric Ferkel, W. D. (2015). Entrapment Neuropathies of the Foot and Ankle. Clinics in Sports Medicine, 791-801
- ↑ Radin, Eric L. "Tarsal tunnel syndrome." Clinical orthopaedics and related research 181 (1983): 167-170.
- ↑ 27.0 27.1 Takakura, Y., et al. "Tarsal tunnel syndrome. Causes and results of operative treatment." The Journal of bone and joint surgery. British volume 73.1 (1991): 125-128.
- ↑ Baba, H., et al. "The tarsal tunnel syndrome: evaluation of surgical results using multivariate analysis." International orthopaedics 21.2 (1997): 67-71.
- ↑ Raikin, Steven M., and John M. Minnich. "Failed tarsal tunnel syndrome surgery." Foot and ankle clinics 8.1 (2003): 159-174.
- ↑ Goldstein, S. H. "Cryosurgery for the Treatment of Tarsal Tunnel Syndrome." PODIATRY MANAGEMENT 25.8 (2006): 163.
- ↑ Wallach, D. M., and S. D. Katchis. "Tarsal tunnel syndrome." Disorders of the heel, rear foot, and ankle. Churchill: Livingston (1999): 125-34.
Created by:
John Kiel on 14 June 2019 08:40:12
Authors:
Last edited:
1 October 2025 19:00:49
Categories:
